Anemia and Iron
Contents
- 1 Introduction
- 2 Why do we need iron?
- 3 How much iron do we need?
- 4 Causes of iron deficiency
- 5 Clinical features of iron deficiency
- 6 How do we diagnose iron deficiency?
- 7 How do we treat iron deficiency?
- 8 Key points
- 9 Anemia Videos
- 10 Table 1: Oral iron preparations
- 11 Table 2: Intravenous iron preparations*
Introduction
Iron deficiency is common among people with HHT and is primarily a consequence of bleeding from telangiectasias in the lining of the nose and intestinal tract. Iron deficiency tends to be both under-diagnosed and under-treated in HHT patients and can lead to decreased exercise tolerance, chronic fatigue, and poor quality of life. The purpose of this article is to highlight the common manifestations of iron deficiency and discuss its treatment.
Why do we need iron?
Iron is required for the production of hemoglobin in red blood cells and the protein myoglobin in muscle cells. Iron is also a component of many proteins and enzymes in the body and plays important roles in energy metabolism and immunity. The total amount of iron in an adult is about 3-4 grams. The majority of this (about 2.5 grams) is present in hemoglobin within circulating and developing red blood cells. About a gram of iron is present as ‘stored iron’ mostly in the bone marrow, liver and spleen. Of note, women of child-bearing age usually have lesser amounts of stored iron, as they use more iron to make up for menstrual blood loss and iron requirements during pregnancy, childbirth and nursing.
How much iron do we need?
The amount of iron in the body is tightly regulated. As the body cannot make iron, the amount of iron absorbed from the diet needs to equal the amount of iron lost on a daily basis. This is about 1mg of iron per day. The daily requirement is slightly higher in adult women (2mg/day) secondary to menstrual loss. The iron requirements are higher during adolescent years due to growth and development. Iron requirements also increase during pregnancy and the total amount of iron utilized during pregnancy, childbirth and nursing is about 1 gram. Foods that are rich in iron include red meats, liver, egg yolk, salmon, tuna and oysters (iron in these foods are in the form of hemoglobin and myoglobin, referred to as heme-iron). Iron is also present is vegetables, fruits and grains, but this iron (referred to as non-heme iron) is harder for the body to absorb.
Causes of iron deficiency
 The overwhelming cause of iron deficiency in developed countries is blood loss. Less likely causes include decreased intestinal absorption (e.g. Celiac disease, following gastric bypass surgery), and decreased iron intake (in extreme diets). Unless an individual experiences sudden and massive blood loss, iron deficiency tends to develop slowly over time. At first, the body progressive uses up its iron stores due to an imbalance between the supply and demand for iron in the body. In this early stage people do not yet have anemia, as there is sufficient iron available for hemoglobin synthesis. However, if the imbalance persists (such as with continued bleeding as can happen in HHT), over time the iron stores become exhausted resulting in iron deficiency anemia. It is important to realize that iron deficiency can occur in the absence of anemia, affected individuals can develop clinical symptoms from iron deficiency even without anemia. This state can be diagnosed using routine laboratory tests.
The overwhelming cause of iron deficiency in developed countries is blood loss. Less likely causes include decreased intestinal absorption (e.g. Celiac disease, following gastric bypass surgery), and decreased iron intake (in extreme diets). Unless an individual experiences sudden and massive blood loss, iron deficiency tends to develop slowly over time. At first, the body progressive uses up its iron stores due to an imbalance between the supply and demand for iron in the body. In this early stage people do not yet have anemia, as there is sufficient iron available for hemoglobin synthesis. However, if the imbalance persists (such as with continued bleeding as can happen in HHT), over time the iron stores become exhausted resulting in iron deficiency anemia. It is important to realize that iron deficiency can occur in the absence of anemia, affected individuals can develop clinical symptoms from iron deficiency even without anemia. This state can be diagnosed using routine laboratory tests.
Clinical features of iron deficiency
The clinical features of iron deficiency are mainly related to anemia and include fatigue, weakness, headaches, irritability, and decreased exercise tolerance. Rarely, affected individuals can develop dry mouth, hair loss, and brittle fingernails. In children and adolescents, iron deficiency (with or without anemia) can also cause poor cognitive function (difficulty with concentration and learning, memory, school performance, etc) and poor physical performance (running, endurance). Further, studies have shown improvement in performance with correction of the iron deficiency. A classic but uncommon finding in individuals with iron deficiency anemia is a craving for ice or substances like clay (referred to as ‘pica’). Iron deficiency has also been associated with Restless Leg Syndrome, a condition causing an urge to repeatedly move the legs or arms because of an uncomfortable feeling in the affect body part.
How do we diagnose iron deficiency?
Iron deficiency should be suspected in any person with HHT who develops one or more of the above mentioned clinical features. Further evaluation should consist of doing the following blood work: a complete blood count (CBC), reticulocyte count, and an iron panel (serum iron, iron saturation, total iron binding capacity, ferritin). These together provide information on a persons iron stores and whether or not an individual is iron deficient/anemic.
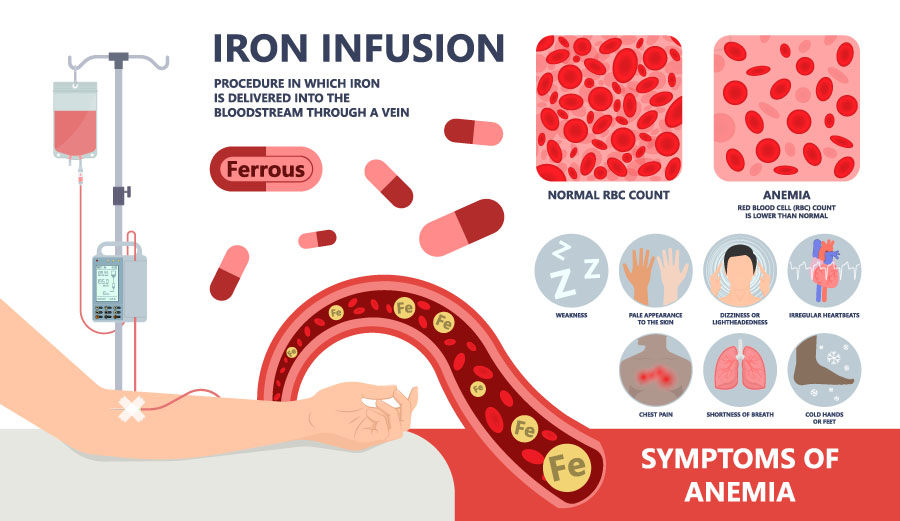
How do we treat iron deficiency?
Once a person has been diagnosed with iron deficiency, this should be corrected by replacing the iron stores. The goal is to correct the iron deficiency as well as replenish the body iron stores. This can be achieved by taking iron by mouth in the form of iron supplements (tablets, liquid, suspension or elixir) or by replacing iron directly into the vein (intravenous or IV). Generally, the initial approach is to pursue oral iron replacement. A number of oral iron preparations are available and some of the common preparations, their trade names and the amount of elemental iron they contain are summarized in Table 1. It is important to note that oral iron supplements can be associated with gastrointestinal side effects such as nausea, bloating, and constipation that frequently limit their use. The side affects appear to be related to the amount of elemental iron and, therefore, preparations that contain less elemental iron tend to be better tolerated. Once the hemoglobin becomes normal, there is still a deficiency in the total amount of iron in the body, and it is recommended that iron treatment be continued for an additional 6 months to replace the missing iron stores in the body.
In individuals with severe iron deficiency anemia or frequent/severe bleeding, oral iron may be inadequate to treat the iron deficiency. In such cases, and in individuals who do not tolerate oral iron, treatment with intravenous iron should be considered. A number of intravenous iron preparations are currently available. The number of doses of intravenous iron necessary to correct a person’s iron deficiency will vary depending on the preparation being used. The currently available drugs and the amount of iron they contain are summarized in Table 2. Of note, preparations that contain less iron (Ferrlicit, Venofer, etc) have the advantage of quicker infusions. On the other hand, the iron dextran preparations (INFeD, Dexferrum) take a few hours to administer but offer the option of replacing the entire iron deficit in a single infusion. Regardless of the preparation used, intravenous iron can be associated with allergic reactions. Some preparations require use of a small test dose and pre-treatment with antihistamines (e.g. Benadryl) for this reason.
Following iron replacement, one can begin to see a rise in the hemoglobin in 2-4 weeks. It is important to realize that treatment with iron, either oral or intravenous, will not immediately correct the anemia. Therefore, individuals with symptomatic anemia may need to receive an initial blood transfusion to improve their symptoms. While transfused red blood cells contain iron (about 250mg/unit of blood), this alone is inadequate to correct the iron deficiency.
It is essential in individuals with HHT who have frequent nose bleeds or intestinal bleeding to continue to aggressively treat/prevent iron deficiency. Once treatment with iron is started, it is important to repeat a CBC and iron panel in 2-3 months to assess response to treatment. Individuals with chronic nose or GI bleeding who tolerate oral iron should continue to take this long term. Individuals that require treatment with intravenous iron may require repeated treatments based on the severity of bleeding.
Key points
- Iron deficiency is an important and under-appreciated cause of symptoms and poor quality of life among individuals with HHT.
- People with HHT who suffer from bleeding should be routinely screened for iron deficiency. The appropriate blood tests for the physician to order are: CBC, reticulocyte count, and iron panel.
- If iron deficiency is found, this should be treated aggressively.
- If oral iron preparations are poorly tolerated or the iron deficiency is very pronounced, iron can be given intravenously in easy to give preparations.
Anemia Videos
Table 1: Oral iron preparations
| Generic names [available formulations] | Product names | Amount of iron (varies depending on the preparation between tablets, liquids, elixirs, etc.) | Comments | |
| Total dose | Elemental iron | |||
| Ferrous gluconate [available as tablets] | Fergon | 240-325mg | 27-38mg | Non-heme iron products.
These products contain higher amounts of elemental iron compared to heme-iron containing products. These are also associated with greater GI toxicity compared to heme-iron products. |
| Ferrous sulfate [available as liquid, elixir, suspension, tablets, timed-release tablets and enteric coated tablets] | Feosol
Slow FE Fer-iron Fer-In-Sol Mykidz Iron |
75-325mg | 15-65mg | |
| Ferrous fumarate [available as regular and timed release tablets] | Femiron Ferretts
Ferro-Sequels Hemocyte Ircon |
63-325mg | 20-106mg | |
| Polysaccharide-iron complex [available as capsule and elixir] | Niferex
Nu-Iron Ferrex-150 ProFe Poly-Iron 150 |
60-180mg | ||
| Iron polypeptide as dietary supplements | Proferrin ES | 12mg | Heme-iron product | |
| Combined heme and non-heme dietary iron supplement | Bifera | 6mg as iron-polypeptide
22mg as polysaccharide-iron complex |
||
Table 2: Intravenous iron preparations*
|
Generic names |
Product names |
Amount of iron per dose |
Duration of dose administration [approximate] |
| Ferric gluconate | Ferrlecit | 125mg | 2 hours |
| Iron sucrose | Venofer | 200mg | 75 minutes |
| Ferumoxytol | Feraheme | 510mg | Rapid infusion |
| Iron dextran# | INFeD [low molecular weight dextran]
Dexferrum [high molecular weight dextran] |
50mg/mL – dose calculated based on weight and hemoglobin to replace total iron stores in a single infusion | 3-4 hours |
| Ferric carboxymaltose@ | Ferinject | 1gram | 15 minutes |
* All intravenous iron products can be associated with potentially life threatening allergic reactions
# High molecular weight carries the highest risk of life threatening allergic reaction, which occur in about 11 per million doses administered. This is less with the low molecular weight dextran (3 per million doses).
@ Not available in the USA