Spinal Cord Injury (SCI) Rehabilitation Reader
 |
 |
 |
| Chair’s Message | Patient Stories | SCI Medicine |
Welcome!
Welcome to our first all-electronic newsletter. You may click on any of the sections (above) to jump to related stories, or you may print the complete newsletter from this page. Additionally, our abbreviated, hard-copy versions are still available when you visit our PM&R Outpatient Clinic or by emailing the outreach editor.
 |
| Dr. Michael Lee |
I am grateful for the excellent leadership of our spinal cord injury (SCI) rehabilitation team.
Dr. Heather Walker demonstrates compassion and knowledge in caring for SCI patients in both our inpatient and outpatient settings. She is committed to this patient population, having pursued a fellowship in spinal cord injury medicine following residency in Physical Medicine & Rehabilitation.
Additionally, our colleagues in the UNC Health Care Rehabilitation Center continue to create new programs benefiting our SCI patients, such as aquatics therapy and an upcoming Spinal Cord Injury Awareness Week. Look for updates about these programs on our website soon.
I also would like to take this opportunity to thank the Stiffler Family for their generous donation. By honoring their loved one, Mr. Herbert Edwin Stiffler, a memorial fund is now available to help our SCI patients who are financially challenged to return home after their injuries.
This fund will be used to make minimal modifications to help patients navigate in and out of their homes independently. If you would like to get involved with this project or make a donation to the department, please contact us.
—Michael Y. Lee, MD, MHA, Professor and Chair of UNC PM&R
►Can you guess where Dr. Lee’s photo (above) was taken? Go to Global Partnership in Medical Rehabilitation to learn about our department’s role in this South American country!
Patient Stories
- Young Wrestling Champion Stays Positive Following a Spinal Cord Injury
- Peer Mentor Brings Renewal to Patients
- Businessman Gives Back, Helps Others with Spinal Cord Injuries
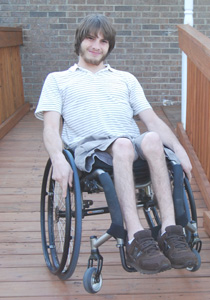
Young Wrestling Champion Stays Positive Following a Spinal Cord Injury
 Bradley Saunders always tackles new challenges.
Bradley Saunders always tackles new challenges.
“I’m a good learner,” he says. “For example, when I started wrestling in ninth grade, everything came naturally.”
During his senior year, Saunders finished first in the region and second in the state, with a record of 119 wins and only 19 losses.
He had never missed a day at his part-time job at Bojangles. He was planning to work in the summer and save for college.
On the evening of his last day of high school in 2007, Saunders felt the victory of imminent graduation while driving with a friend in his Celica Supra, when suddenly his life took a turn.
“I was speeding, coming home from the swimming pool on a back road,” he recalls. “We hit a dip in the road, and I lost control of the car.”
Saunders, who was conscious the whole time, thought his friend had landed on top of him. His back hurt and he couldn’t feel his legs. He called out, “Get off me,” but his friend answered him from the woods outside the car. Saunders then looked closely at the shoes above his head: they were his own.
Still unable to move his legs, Saunders nevertheless pulled himself from the upside-down car to join his friend outside. (Luckily, his friend had sustained only scrapes and bruises.)
Thankfully, a stranger stopped to call for rescue. “I still don’t know who he was,” Saunders says, “But he saw the whole accident happen.” Saunders’ best friend also happened to drive by the accident, and recognized the car’s tires. In no time, his family and his neighbors — some of whom were part of the rescue team — comforted him as he was loaded onto a stretcher. “The medics were rushing me to UNC Hospitals, because they knew there was a severe injury to my spine,” Saunders explains.
After surgery for his broken back, Saunders remained paralyzed from the waist down. He came to the UNC Health Care Rehabilitation Center to learn how to keep adapting and improving. With the help of George Atkinson, MD, a rehabilitation doctor (physiatrist) in the UNC Department of Physical Medicine & Rehabilitation at that time, and other members of the rehabilitation team, Saunders returned home after intensive therapy.
“Bradley had his rough days like everyone else,” Dr. Atkinson recalls, “but he always tried to do his best.”
Saunders also credits the interdisciplinary rehabilitation team. “You learn shortcuts that work for you as an individual,” he says, fondly recalling how he learned forward and backward “wheelies” off the curbs in the hospital parking lot with therapists Wes Hudson, PTA, Kevin Corbin, OT, and Courtney Matrunick, DPT.
“They teach you how to maneuver a wheelchair when you don’t have accessibility,” he explains.
Jason DeLuca, MD, then a resident in the UNC Department of Physical Medicine & Rehabilitation, came to check on Saunders one night after work, at
11:00 PM, to be sure Saunders was “doing OK” after a rigorous day. “That really meant a lot to me,” Saunders says.
 |
| Saunders credits his new patience for helping him shoot his first buck. After hunting, he prepares deer jerky for himself and his family. |
Thanks to family and friends, Saunders came back to a wheelchair-accessible home, complete with a new ramp. The community of Snow Camp has hosted a number of fund-raisers to help pay the balance of medical costs not covered by insurance. Susan Carter, RN, CRRN, and Misty Townsend, RN, two nurses from the Rehabilitation Center, also attended the fundraisers.
“We found out that several of our neighbors are paralyzed,” says Saunders’ mother, Jeannie Saunders. “One of them invited Bradley to come over to see how he has made his house accessible.”
“We have had wonderful support,” she notes. C.T. Nassau of Burlington, the company where she works, gave her a temporary leave of absence to care for her son until he became more independent. Saunders’ older brother, David Saunders, continues to stretch him daily and provide transportation when needed.
 |
||
|
Saunders and his father, Ronald Saunders, recently resumed hunting in the Virginia mountains. “I couldn’t get up and move the way I used to,” Saunders says. “That made me more patient; I was able to shoot my first buck.”
Saunders continues to provide hope to others with his unfailing smile. “I’m lucky to be alive,” he says. “That’s why I’m smiling.”
“Driving that fast should have killed me, but it didn’t. That shows you anything can happen,” he adds. “Will I speed again? Probably not. Will I walk again? I believe I will, either with new advances in medicine or with my own learning.” Saunders meanwhile continues to tackle his short-term goals, such as securing a full-time job and learning to drive with adaptive equipment.
As our interview draws to a close, Saunders demonstrates one of his “wheelies” as he ventures outside his parents’ house. He proceeds to enjoy fresh air and conversation with his mother on the porch.
“We’ve always been close,” Jeannie Saunders says as she sits beside her son. “In that sense, nothing has changed.”
Peer Mentor Brings Renewal to Patients
 |
|
Tal (right) and Kelly O’Brien, speech therapist, meet to discuss Tal’s guitar-playing in upcoming sessions.
|
“I was delighted to hear about the Peer Mentor Program,” says Gabriella Tal. “While I was in the hospital after my spinal cord injury fourteen years ago, I met a man in a wheelchair named Del Spruill who was like a peer mentor for me. He helped me immensely and we stayed friends for many years.”
After Spruill’s passing, Tal felt a push to give back, and the Peer Mentor Program turned out to be the perfect fit.
“Sometimes it’s as simple as showing someone how to transfer, or giving a reference of people who build ramps. That’s the practical difference I can make,” Tal relates. “For emotional support, laughing together is a very transformative thing. You could be crying, but you end up laughing. Or, if you are in grief, it’s easier to hold the hand of a person who has been there.”
Tal’s larger message shines through: “I encourage people to be careful consumers, with all the new research out there. In the meantime, you have to live your life, even if you believe, as I do, that a cure for SCI will come in our lifetimes.”
Tal shares stages she went through, after feeling she had given up something essential in walking. She describes how she struggled to reclaim parts of her former life, and to “relearn everything again,” this time from the vantage point of living in a wheelchair.
“For several years after my accident, I had a caregiver, and lived in an apartment,” she remembers. “I had always loved nature, so I put potted plants on the balcony. When I became more independent, I was able to move out to the country again, back to nature.”
“It takes courage to get in a wheelchair and face life,” she continues. “There are pot holes to avoid, toilets to get on and off, showers to get in and out of, airplanes to navigate. I have a T12 SCI, which means I have all my upper body, and my stomach muscles. If a person has a higher SCI, they have an even more difficult road.”
“I’m in awe of the patients, and feel a deep kinship and respect for what they’re undertaking,” she notes. “I also was blown away by the staff at the UNC Rehabilitation Center, from the front desk to the PTs to the nurses to the people who bring the food. This is a hard place to work, because there is a lot of pain and suffering. The staff and volunteers bring light into dark places.”
 |
|
| Phil Austin (left), a PM&R patient and volunteer, advises and supports Tal (right) in her role as a new peer mentor. |
“I’ve been privileged to be supervised by Phil Austin,” Tal adds. “He’s a stroke survivor and a model of compassion; he has a brilliant awareness of how to be with people. As a teacher, he gives support, but leaves room for me to find my own strength as a peer mentor. All of us do things a little differently, but I aim to follow his example of empathy for the patients.”
Tal helps a variety of SCI patients, and others, by seeing similarities in their concerns. “It’s a new life in so many ways for all of them,” she says. “They all have had some kind of serious shock and change, and often a huge loss. They ask: ‘How can I do it?’ It took me years to fully accept and adapt to my situation, and finally to thrive. I encourage them not to give up.”
Tal also is a massage therapist, body-mind therapist and clarity therapist practicing in Chapel Hill. You may reach her via email or visit her website for more information.
Congratulations on Program Growth!
The Peer Mentors Program (formerly the Stroke Mentors) now helps all patients at the UNC Health Care Rehabilitation Center. Congratulations to Karla Thompson, PhD, program director, and our wonderful volunteers for completing this expansion to help more patients.
Businessman Gives Back to UNC, Helps Fellow Patients with Spinal Cord Injuries
 |
| Travis Blake |
Travis Blake appreciates the many second chances granted to him from UNC. That’s just one of the reasons he gives back.
At NC Building, his sustainable development and construction firm south of Chapel Hill, he finds time to volunteer and raise money for the UNC Department of Physical Medicine & Rehabilitation, even amid the buzz of phone calls, messages from other associates, and the darting of an enthusiastic puppy from one office to another.
Blake and other generous partners are contributing time and finances for a project to help others with spinal cord injuries. Patients who recently have stayed at the UNC Rehabilitation Center, and who demonstrate a need for ramps or other accommodations, may apply to be considered for modest renovations to ease the return home.
Additionally, Blake is working with UNC to create a credentialing program for nursing home managers. He also began a new business direction, called TLC, which brings an array of services allowing older adults to remain at home.
Blake stays busy, partly because he knows the importance of returning home, and improving one’s own opportunities, after a severe injury: In May 1976, Blake’s motorcycle swerved around a sharp curve and down a bluff near the Chapel Hill Tennis Club. He subsequently spent four months at UNC Hospitals with neck and spine injuries, and was permanently disabled as an incomplete quadriplegic.
“A lot of people don’t know that much about themselves until something like this happens,” Blake says. “I had been an athlete, and had relied on that strength. Fortunately, I learned that I also had a strong mind.”
Prior to his accident, Blake had dropped out of UNC several times, due to business successes out of school. After the accident, however, Blake eventually earned three degrees at UNC: a Bachelor’s Degree in Biology, Bachelor’s of Science in Public Health, and a Master of Public Health in Environmental Sciences and Engineering; he also attended Duke towards earning his PhD. “I had to break my neck to get back in school,” Blake laughs.
“Obviously my condition is complicated, especially as I age,” Blake says. “It was wonderful meeting Dr. Lee some years ago and knowing there was a whole department set up to follow patients like me.”
Michael Y. Lee, MD, MHA, professor and founding chair of the Department of Physical Medicine and Rehabilitation, manages Blake’s care as a rehabilitation physician (physiatrist) working with various medical specialists.
“The doctors at UNC think differently; they do research that many times can help patients have a much better chance of recovery,” Blake notes.
For more information about applying for or contributing to spinal cord injury funds, contact Nicole Pratapas via email or call 919.966.8494.
Spinal Cord Injury Medicine
- Physiatrists: Critical Professionals for Spinal Cord Injured Patients
- Therapists Prepare SCI Patients to Re-Enter Communities
- Reflection on a Home Visit to the Saunders Family: By George Atkinson, MD
- More Information and SCI Resources
Physiatrists: Critical Professionals for Spinal Cord Injured Patients
Heather Walker, MD, a rehabilitation physician (physiatrist) in the UNC Department of Physical Medicine & Rehabilitation, completed a post-residency fellowship in spinal cord injury medicine at the Kessler Institute for Rehabilitation. Nationally board-certified in both PM&R and Spinal Cord Injury Medicine, she manages a host of issues related to spinal cord injury (SCI) over the course of a lifetime.
 |
| Dr. Heather Walker |
One of the top concerns following injury is management of bowel and bladder, as well as other secondary complications. Depending on the severity of the injury, communication between nerves supplying the bowel and bladder and the brain can remain blocked, causing individuals to be unable to perform these functions voluntarily. Most people with an SCI will require medications to assist with bowel evacuation, and they also will need a method to drain their bladder.
“In the past, kidney failure was the leading cause of death in individuals with SCI. Thankfully, kidney disease now can be prevented in SCI patients with appropriate management,” Walker notes. “When patients with new SCI are admitted to inpatient rehabilitation, we educate them on different methods for bladder management, and with the assistance of the rehabilitation nurses, the patients are able to learn the appropriate techniques.”
Dr. Walker also coordinates care with other medical professionals, such as a urologist. “Individuals with an SCI should be seen by a urologist for basic testing, including a renal (kidney) ultrasound, blood work and urodynamics within a few months after their injury, and then on a yearly basis,” she advises.
Even in these modern times, SCI patients still need to watch for signs of a potentially life-threatening secondary condition known as autonomic dysreflexia. The condition usually arises with an interruption to the bowel/bladder routine and often causes a steep rise in blood pressure. It occurs primarily in patients with SCI at the T6 (mid-torso) level or above, and it is more common in individuals with a neurologically complete SCI. (A complete SCI means lack of sensory and motor function below the level of injury, as opposed to an incomplete SCI, which allows some function below the injury).
“Many physicians in the community may not know about autonomic dysreflexia,” Walker says. “That’s why we educate rehabilitation patients who are at risk for this condition on the common symptoms and appropriate initial management for autonomic dysreflexia. We advise them to seek immediate medical help if they are unable to resolve the episode.” For more information, Dr. Walker also recommends Paralyzed Veterans of America: http://www.pva.org
Ideally, SCI patients would visit a physiatrist such as Dr. Walker at least once a year, for management of these and other secondary conditions. Other issues following SCI include spasticity (spasms), pressure ulcers/skin breakdown, mood disorders, and equipment needs such as wheelchairs, cushions and bracing, among others.
“Spasms can be very painful and can interfere with patients’ function,” Walker notes. “If spasticity is not addressed, it can lead to contractures that may require surgery.” Dr. Walker manages spasticity in the PM&R outpatient clinic with oral medications, and in appropriate patients she administers EMG-guided botulinum toxin injections. These injections offer a precise, non-surgical intervention for focal spasticity and are a good option for patients who do not tolerate the side effects of oral medications.
 |
| Dr. Tracy Kent |
Tracy Kent, MD, a fourth-year resident in the department, has been learning from Dr. Walker about preventative strategies as well as state-of-the-art advances that lend more mobility to SCI patients. “Even if a patient has no mobility in the arms and legs, as a complete quadriplegic, he or she can use a special straw to control wheelchair movement,” Kent observes. “A patient can sip, or blow, to control direction.”
Dr. Kent also hopes to emulate her mentor’s good relationships with patients. “Dr. Walker is very understanding and compassionate,” she notes. “At the same time, she can see the whole picture: she knows exactly what each patient needs.”
“Once, we had an SCI patient come to our outpatient clinic,” Kent recalls. “He hadn’t seen a doctor for some time, so unfortunately he had every secondary condition you could imagine. Dr. Walker immediately got him into our rehabilitation center as an inpatient and coordinated other care to aid in his recovery. That’s when I realized the difference physiatrists can make: we are the only doctors trained specifically in SCI.”
Drs. Walker and Kent, along with other colleagues and generous donors, are developing a program for newly injured SCI patients who are financially challenged. They hope to assist with minor home modifications that will make it possible for individuals to return home. For more information, please contact Nicole Pratapas via email or at 919.966.8494.
Therapists Prepare SCI Patients to Re-Enter Communities
“We try to bridge the gap between the hospital and the real world,” says Kelly O’Brien, MA, CCC-SLP, a clinical speech pathologist in the UNC Health Care Rehabilitation Center. O’Brien gives patients critical tools and support for swallowing and communication, which some spinal cord injury patients require, and helps coordinate a weekly aphasia (communication) support group.
When O’Brien helps a patient increase the “volume” of his or her voice with breathing exercises, for example, this not only increases confidence at the time, but also provides an additional step toward more independence in the community.
Increasing vocal quality is one of many skills patients may need to re-learn after their injury. Speech, physical, occupational and recreational therapists help patients maximize their potential for a new life.
Courtney Matrunick, DPT, a doctor of physical therapy at the Rehabilitation Center, teaches patients with spinal cord injuries (SCI) compensatory strategies for functional mobility. People with spinal cord injuries need to learn how to find their new balance point after their injury, and Matrunick and her colleagues facilitate this process.
“It’s essential to have a good understanding of anatomy and how the body moves normally,” Matrunick notes. “For example, if you hold your forearm up and let your wrist drop forward, your fingers naturally straighten. Letting your wrist fall back causes them to naturally bend. This can be helpful for those without finger strength to grasp things like a cell phone.”
“Even if patients are unable to push through their arms, we can teach them how to lock their elbows for more controlled movement,” Matrunick continues.
Therapists stay in constant communication to guarantee they address individual patient needs and work toward the same goals. “Working together, we help patients regain their life,” Matrunick adds. “It’s exciting to make a huge difference.”
“I see infinite potential in people living with spinal cord injuries” says Raheleh Tschoepe, OTR/L, an occupational therapist at the Rehabilitation Center. “I can teach them a new way of living as they take on a new identity and a new role.”
She recalls teaching her patient, Bradley Saunders, how to use adaptive equipment for dressing and bathing. “When he returned home, he also used this equipment to pick apples from a tree,” she notes. “We empower patients to think outside the box; that’s what we hope for.” (See related story about Bradley Saunders.)
“To be the educator is as much responsibility as being the recipient,” Tschoepe adds. “You have to be thorough but not overwhelming.”
Therapists also are advancing SCI care at UNC by enhancing patient education resources, offering outings for aquatic therapy, and hosting SCI Awareness Week in Fall 2009.
Therapy is only one part of successful rehabilitation. The patient’s potential lies within the integration of the physician’s guidance, nurses’ diligence in care, psychological support and family encouragement.
►Stay tuned to our website for upcoming information on SCI Awareness Week in Fall 2009. For more information about support groups for aphasia and brain injury following SCI, go to Local and Global Outreach.
Reflections on a Home Visit to the Saunders Family
Article by George Atkinson, MD
Editor’s Note: George Atkinson, MD, is a former resident of UNC PM&R who also served as a faculty member from 2007-2009. He has since moved back to his home state of Texas to continue as a physiatrist.
House calls are something I’ve always wanted to do. I thought I might learn something new, seeing how Bradley Saunders functions in his home environment, beyond the clinic setting.
I was excited and nervous on the drive to Bradley’s home, not knowing what to expect. That made me understand how patients and family might be nervous coming to see me in the clinic. Now the tables were turned!
On my drive there, however, I relaxed more and more as I viewed the countryside. I thought: Bradley lives in a tranquil, serene place. Bradley and his mom were there to greet me, so I was completely at ease by that point. I was the one happy to be greeted in a welcoming atmosphere! I thought about this as I sat down on the couch about to ask some questions – the importance of being comfortable enough to ask questions.
 |
| Dr. Atkinson (left) with Bradley Saunders and his parents, Jeannie and Ronald Saunders |
I asked how Bradley was functioning in the house. (I had noticed the ramp and the appropriate, safe entryway.) I asked how he goes in and out of the bathroom. He excitedly showed me adjustments the family had made. For example, the cabinet under the sink was removed so his legs could fit, and the family didn’t mind this practical adjustment.
He then showed me how he gets in and out of his room, and I was impressed with all his awards from his wrestling career in high school. He and his parents were very proud of the awards, and we had a good discussion about what he had done in the past. This was a good time to reiterate that he could certainly stay active and independent. I encouraged him to follow his dreams. I thought: he should be able to do whatever he wants. I became the advocate turning the conversation!
I got a chance to talk more than in the clinic, so I learned about issues Bradley had been dealing with such as finding permanent work and getting his driver’s license with adaptive equipment. I thought: he needs to have adaptive equipment because he’s a very motivated individual. It’s almost like a chicken and egg problem, and it was important for me to learn how these issues affect Bradley’s life.
I learned just how appreciative the family was having their physiatrist go out to the home. The visit had a larger effect than I had anticipated. I think the home visit will make Bradley’s clinic visits more efficient in future. He will be able to resolve some issues more directly, because he had the opportunity to feel more at ease with a doctor.
Putting in the time to go to a patient’s home lends insights that can help other patients. For example, I’m thinking more about community advocacy and looking for solutions. I certainly would be interested in making more house calls in the future.
For more information…
►Would you like to subscribe to this newsletter via email? Sign up on our Rehabilitation Reader listserv!
►For general information about our department, browse the rest of our website or contact us at UNC PM&R.
►For more about spinal cord injuries, including statistics & prevention, visit the following website:
http://www.nlm.nih.gov/medlineplus/spinalcordinjuries.html
