Project III: Models of Human Smoking-related Diseases: What is the Best Mimic of Human Disease?
Tobacco smoke is the most common cause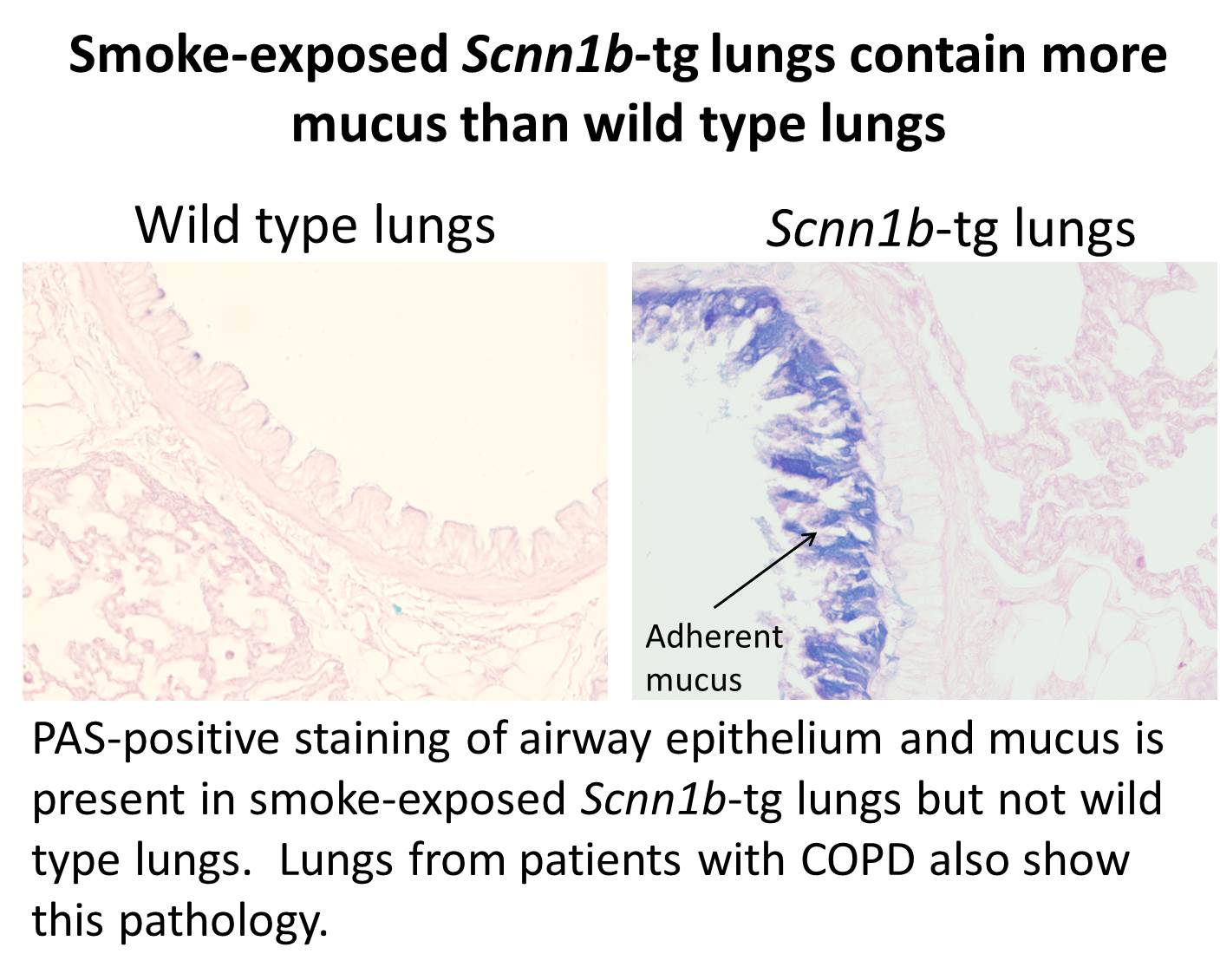 of chronic obstructive lung disease (COPD). Most laboratory models of tobacco smoke related lung disease result in mild-to-moderate emphysema, but with little or no evidence of chronic bronchitis, a large component of COPD in humans. Recently, we began modeling tobacco smoke exposure by exposing airway epithelia overexpressing Scnn1b, the gene that codes for the epithelial Na+ channel subunit (βENaC), to tobacco smoke. These initial studies suggest that this model mimics human injury more closely than previous models. This
of chronic obstructive lung disease (COPD). Most laboratory models of tobacco smoke related lung disease result in mild-to-moderate emphysema, but with little or no evidence of chronic bronchitis, a large component of COPD in humans. Recently, we began modeling tobacco smoke exposure by exposing airway epithelia overexpressing Scnn1b, the gene that codes for the epithelial Na+ channel subunit (βENaC), to tobacco smoke. These initial studies suggest that this model mimics human injury more closely than previous models. This 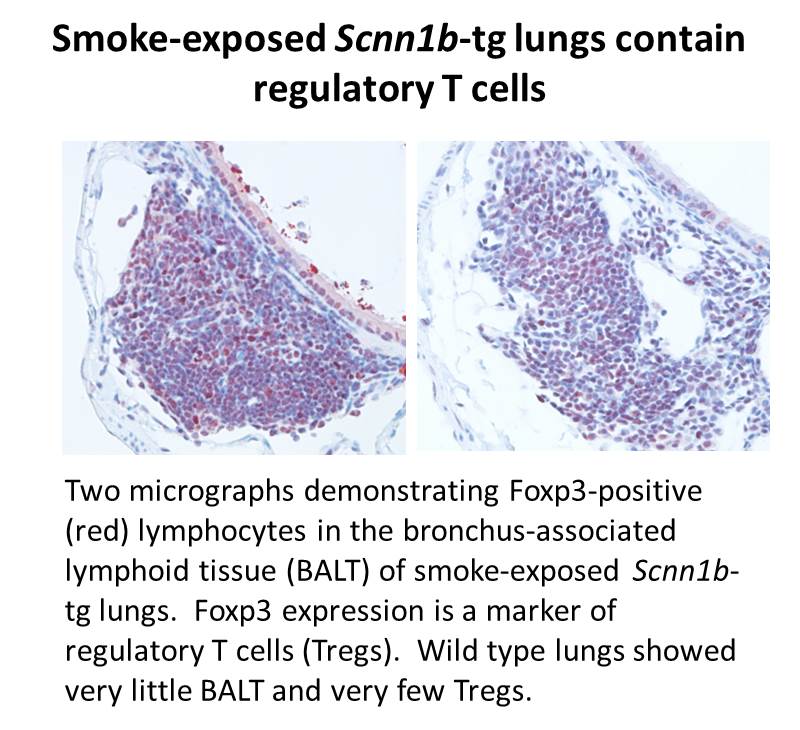 project will test the hypothesis that smoke exposure of lungs with Scnn1b-overexpresssing epithelia is an excellent model of human disease and can be used more effectively than other models to study particular tobacco products or substitutes.
project will test the hypothesis that smoke exposure of lungs with Scnn1b-overexpresssing epithelia is an excellent model of human disease and can be used more effectively than other models to study particular tobacco products or substitutes.
The first aim of this project is to establish this model by exposing Scnn1b-overexpresssing and wild type airway epithelia to tobacco or sham smoke and analyzing the following parameters related to disease: (i) pulmonary immune cell populations and cytokine production; (ii) immunophenotypes of cells in the lungs and mediastinal lymph nodes; (iii) protein and miR content of mucus and airway exosomes; (iv) mucociliary clearance and clearance of H. 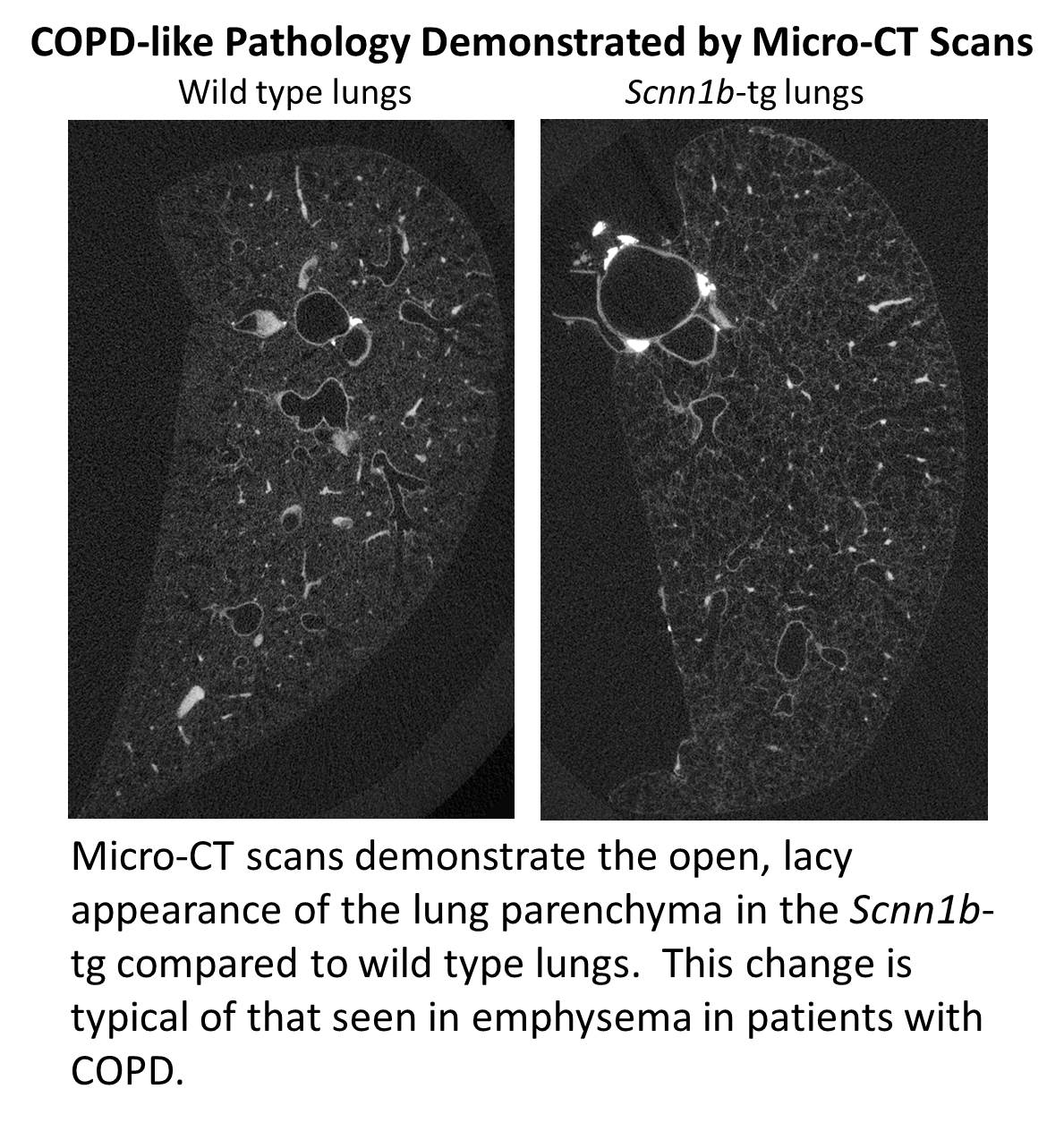 influenza; (v) mRNA and miR expression in whole lungs and isolated lung cells, including macrophages, neutrophils, and epithelial cells; and (vi) the activity of five critical intracellular signaling pathways in epithelial cells including the NF-κB pathway and the Keap1/Nrf2 pathway using bioluminescent in vivo reporters.
influenza; (v) mRNA and miR expression in whole lungs and isolated lung cells, including macrophages, neutrophils, and epithelial cells; and (vi) the activity of five critical intracellular signaling pathways in epithelial cells including the NF-κB pathway and the Keap1/Nrf2 pathway using bioluminescent in vivo reporters.
We will then compare these results to the data generated from our human studies and from the literature to define the degree of similarity between our model of tobacco smoke-induced lung injury and disease seen in humans. We will then be able to determine the adverse health consequences of new and emerging tobacco products (NETPs), such as little cigars and  hookahs, using the same parameters listed above and compared these results to those generated from our cigarette studies to help fully define the adverse health consequences of NETPs.
hookahs, using the same parameters listed above and compared these results to those generated from our cigarette studies to help fully define the adverse health consequences of NETPs.