Diagnosis
Men account for less than 1% of diagnosed breast cancers in the United States. Per the Breast Cancer organization, “in 2020, 2,620 men are expected to be diagnosed with the disease, and an estimated 520 men are expected to die from breast cancer. For men, the lifetime risk of being diagnosed with breast cancer is about 1 in 833.”

While the risks are low, there is still a possibility of developing breast cancer. That possibility became very real for John Ozols, who at 72 had settled comfortably into retirement. At 6’6”, a retired engineer living in Seneca, SC, his days included doing work around the house, his love for puttering in full force.
It was December 2014. After a day working up a sweat doing chores around his home, he sat down for some water and scratched in itch on his left pec. As he touched his chest, he felt a lump. John wasn’t concerned at first because, over the years, he had experienced fatty deposits on other parts of his body and chalked it up to that. However, John also considered that he’d had an inverted nipple for the last few months. To be safe, he called his brother, Robert Ozols, a retired nationally renowned medical oncologist to ask for some advice.
“My brother didn’t want me to take any chances,” recalls John. “He recommended I get it checked out immediately and go for a biopsy. It turned out he was right because the test came back positive for cancer.”

The word cancer is a general term. Uttering it though can have a profound impact on an individual. Many years ago, its diagnosis would have been the beginning of the end for a patient. Today medical science has come leaps and bounds with options available to treat the disease.
“When I first found out,” John says, “when they told me it was the big C, I thought about what my parents used to say to me, that it was an automatic death sentence. For about a week, I stayed quiet and was at peace that I was going to die but decided it wouldn’t be without a fight. I remembered something my Dad used to say: ‘an intelligent person learns to live with the ever-changing circumstances of life.’”
After coming to terms with his diagnosis, John called his brother with the news. They discussed the situation, and John let Bob take the lead on finding the right institution that could help him with the fight for his life.
“We have a small hospital where I live,” John says. “I consider myself a medical snob. I wanted the best doctors I could find. My brother has a lot of respect for Dr. Hyman Muss, a medical oncologist with UNC, and he suggested I go there for my treatment. He thought they could provide me the best care, and it certainly turned out that way.”
Finding his way to UNC
Once the diagnosis came back, John’s brother called Dr. Hyman Muss, the Mary Jones Hudson Distinguished Professor of Geriatric Oncology and the Director of the Geriatric Oncology Program at UNC.
“Bob is a terrific guy, and we’ve known each other for years from our work in a national Gynecology Oncology Group,” explains Dr. Muss. “When his brother was diagnosed, he gave me a call and we talked. Soon after hanging up with Bob, I spoke to John myself to get a handle on the situation. We got John set up for appointments with our outstanding multidisciplinary team of doctors here at UNC.”
The first appointment John had was with Dr. Kristalyn Gallagher, Section Chief of Breast Surgery and the Surgical Director of the Breast Care Program at UNC. Dr. Gallagher confirmed the diagnosis of breast cancer with John and walked him through his options. “One of the benefits of cancer care at UNC is that every patient will receive a multidisciplinary approach to their care. The breast tumor board meets regularly to discuss all new breast cancer cases and gives recommendations to provide a tailored, personalized approach for every patient.” For John, she recommended proceeding with mastectomy.
The operation and recovery
The operation took place in February of 2015. “I remember sitting in the room, waiting for my surgery to begin. Dr. Gallagher came into see me and she marked up my breast. I remember watching her and asking her if she was a reincarnation of Van Gogh. We laughed and the next thing I remember I was in recovery.”
John’s surgery went well, and he was able to head back to South Carolina shortly after his recovery. He returned later for his follow-up visit and to have the drain tube removed. “During the mastectomy procedure, a drain tube is inserted under the skin to prevent fluid from collecting in the space where the breast used to be.” explains Dr. Gallagher. “The more active a person is, the longer it takes for the volume of fluid to be low enough to safely remove the tube.” John’s tube had to stay in for several weeks. Even after it was removed, he continued to have some fluid build up under the skin and Dr. Gallagher later had to make a small incision to drain the liquid. Dr. Gallagher reviewed the specifics of John’s pathology report and arranged a follow-up with Dr. Muss to discuss additional treatment.
Based on the findings, Dr. Muss felt that John would not benefit from chemotherapy. Instead, he was prescribed Tamoxifen, a drug used over the last 40 years to treat hormone-receptor-positive early, locally advanced breast cancer. It’s to help prevent the disease from recurring.
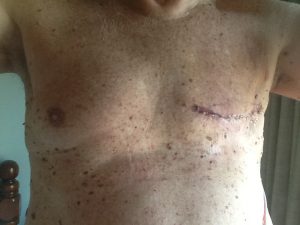 Two and a half years after his surgery, John returned to Dr. Gallagher with another growth under his left pec at the same area where the incision had been made. A needle biopsy was done, but unfortunately there was not enough tissue to make a conclusive diagnosis. There was concern that this could be a second type of cancer as the biopsy showed abnormal cells.
Two and a half years after his surgery, John returned to Dr. Gallagher with another growth under his left pec at the same area where the incision had been made. A needle biopsy was done, but unfortunately there was not enough tissue to make a conclusive diagnosis. There was concern that this could be a second type of cancer as the biopsy showed abnormal cells.
“When there is not enough tissue to be conclusive with a needle biopsy, the next step is to go back to the operating room to obtain a larger sample of tissue. In John’s case, we took him back and removed the growth completely,” says Dr. Gallagher. “When we sent it for testing, the results came back negative. It was a buildup of scar tissue from the original incision we made to drain the liquid years before. We were ecstatic that we could provide him the good news.”

Still today, John has no evidence of cancer. He is enjoying his retirement and puttering around the house. “What I liked about UNC was the multidisciplinary approach,” he says. “I was delighted to meet Dr. Gallagher, and she was a fantastic surgeon. Life is very precious to me. I want to keep living and keep the cancer at bay. I think the world of UNC and all of the people that were a part of my care. It’s been a good journey.”
Breast cancer in men
Many people assume that because men don’t have breasts, they can’t get breast cancer. However, the reality is that all men and women, boys and girls, have breast tissue.
“I talk openly to people about my diagnosis,” shares John. “I never try to cover it up. It’s a fact of life. I didn’t equate it as anything feminine. I’m an exceptional person. I’m in the 1% of men diagnosed with breast cancer.”
As far as medical treatment, there are some nuances of working with a male breast cancer patient as compared to female breast cancer patient. “Doctors treat men similarly, but I think that men that get breast cancer are a little sheepish about it,” says Dr. Muss. “You never see a man showcased with breast cancer; none of the posters or ads talk about it. In the locker room, when you see a man with a chest scar, you never assume breast cancer. Many men feel like it’s a woman’s disease, so I think they feel it’s perceived as a woman’s cancer. While woman are primarily diagnosed, it’s still important for men to be aware that it can happen to them too.”
Like Dr. Muss, Dr Gallagher’s experience with male breast cancer patients is similar. “Most men I have encountered with breast cancer are surprised and tell me they didn’t realize that they could ever get breast cancer. Even though it is rare, it does happen. It is very important to report any changes in your breasts to your physician early. Things to look for are any new or changing lumps/bumps in the breast, nipple discharge, redness, scaling, or bleeding of the nipple in the absence of trauma,” explains Dr. Gallagher. She goes on to say, “It is important for men to know that they have options when it comes to surgery. Men, similar to women, may be candidates for lumpectomy (removing only the area of the cancer and leaving the rest of the breast intact). This decision is dependent on the size and position of the cancer in the breast and their willingness to undergo additional treatment such as radiation. They will also need mammograms in the future to follow the breast tissue that remains. Because male breast cancer is rare, it is also very important for them to be considered in clinical trials so that we can expand our knowledge to best treat male breast cancer.”
“I am so happy that John has chosen to share his story and be a voice for male breast cancer survivors,” says Dr. Gallagher “He has such a positive disposition on life and truly has the mind of an engineer, always wanting to figure out exactly how it works. Not everyone has a family member who can help guide them to the next step and I hope that John’s story can help other men who may be facing a similar situation.”