Dr. Raj Kasthuri talks about hereditary hemorrhagic telangiectasia, also known as HHT, with Dr. Ron Falk. Dr. Kasthuri describes the symptoms, how it can affect internal organs, and treatment for HHT. They also discuss some of the reasons that many people who have HHT are not aware of what they have. Dr. Kasthuri is an Associate Professor of Medicine in the Division of Hematology and Oncology, and he serves as the Medical Director for the UNC HHT Center of Excellence.

“Only about two out of ten people with HHT know what they have…There’s a long way to go in terms of raising awareness, so patients understand what they have.
A big part of this is also educating providers. Even if a patient does the right thing, goes to a physician and says, ‘I’ve got all these problems,’ if the physician cannot make the diagnosis of HHT, then we’re going in circles. So, awareness—both providers and patients—is one big challenge.”
– Dr. Raj Kasthuri
Ron Falk, MD: Hello, and welcome to the Chair’s Corner from the Department of Medicine at the University of North Carolina.
This is our series where we discuss different genetic diseases with physicians who treat patients with these conditions. Today, we will talk about HHT, hereditary hemorrhagic telangiectasia.
We welcome Dr. Raj Kasthuri, who is an Associate Professor of Medicine in our Division of Hematology and Oncology, and he serves as the Medical Director for the UNC HHT Center of Excellence. Dr. Kasthuri helps many patients who have this disorder. We’re going to use the acronym “HHT,” because it’s easier to say than hereditary hemorrhagic telangiectasia. Welcome, Dr. Kasthuri.
Raj Kasthuri, MD: Thank you.
Prevalence and symptoms of HHT
Falk: What is HHT? What is hemorrhagic telangiectasia, or HHT?
Kasthuri: HHT, as you said, hereditary hemorrhagic telangiectasia, also used to be called Osler-Weber-Rendu disease. Now, we’ve changed the name to conform more to what people experience when they have HHT. Hereditarystands for something that runs in families and is inherited. Hemorrhagic stands for a tendency to bleed, and telangiectasia comes from the Greek word where telosmeans “end,” and angion means “vessel,” and ectasiais “dilation.” So, put that together, and you get a dilated blood vessel. What HHT is, is a disorder that runs in families where affected people have dilated blood vessels that tend to bleed.
Falk: How common is it?
Kasthuri: One in five thousand people, we believe, have HHT worldwide.
Falk: That’s a lot. Is it more in some populations than in others?
Kasthuri: It has been described to be more than one in five thousand in some parts of the world, in northern Europe, but there isn’t a propensity within any one country or any one race. HHT occurs in everybody.
Falk: How common is it in the United States?
Kasthuri: The same one in five thousand would put it at about seventy-thousand people with HHT in the United States.
Falk: Is there an increased prevalence here in North Carolina, or is it just as common here or not as common as it is anywhere else? Is it equally dispersed, in other words, in the United States?
Kasthuri: We believe it is equally dispersed in the United States, and that would put about 1,500 to 2,000 patients with HHT in our state.
Falk: What does somebody feel like? What are the symptoms of somebody who has HHT?
Kasthuri: The cardinal symptom of HHT is nosebleeds. The nosebleeds are a result of these abnormal blood vessels that develop. When these blood vessels happen in the lining of the nose, then with irritation, they develop nosebleeds. The tricky part of HHT is, even though it is inherited, it tends to show itself with age. It tends to have an age-dependent expression, so it can be very tricky making the diagnosis in children.
Falk: Wait a minute. It is an inherited disorder that is picked up later in life?
Kasthuri: That’s correct.
Falk: Why? Do the blood vessels dilate over time? What happens?
Kasthuri: They tend to develop over time, and the average age of onset of nosebleeds is estimated to be somewhere in the mid-teens around the ages of fourteen, fifteen.
If you take a fourteen-year-old, and they develop nosebleeds, the first five things that come to mind are probably not an inherited genetic disorder. So, it is not until later on in life when the bleeding gets more severe, and they start to develop these abnormal blood vessels more obviously, over their skin and their hands, the fingertips, around the nails, around the lips, that people start to think about HHT.
Falk: What does a telangiectasia really look like?
Kasthuri: A telangiectasia is a small, red or purple pinpoint lesion—or it can be a cluster—and it classically blanches, meaning, when we put pressure on it, it will disappear. Once you release the pressure, it blushes back on. That’s a classic telangiectasia.
Falk: They can occur on the face, on the hands—where else do they happen?
Kasthuri: They classically tend to happen on the face, over the hands, in the lips, on the lining of the mucosa in the mouth—so you can see it on the tongue, you can see it on the lining of the mouth, the roof of the mouth, over the earlobes.
Falk: Brain?
Kasthuri: Yes.
Falk: Lungs?
Kasthuri: Yes.
Falk: Heart?
Kasthuri: Not heart. It is very interesting, and we haven’t quite figured out why this is, but outside of the skin and mucosal lining, HHT likes to involve only select internal organs. It affects the brain, it affects the lungs, it affects the liver and the GI tract in that the lining of the GI tract can also develop these spots and they can bleed too, causing GI bleeding.
Falk: What happens in the lung? What are the symptoms in the lung?
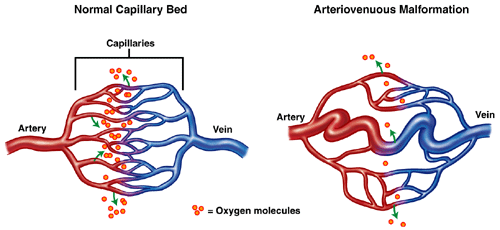
Kasthuri: The internal organ involvement with HHT is very similar to what happens over the skin, which is patients develop abnormal blood vessels. When these develop in internal organs, we call them “arteriovenous malformations,” or AVMs.
Everything that happens in the lung with HHT is because of these AVMs. What happens when blood passes through an AVM is —because these are dilated blood vessels—they do poorly at exchanging oxygen and carbon dioxide. So, any blood that passes through an AVM leaves the lung with carbon dioxide and not oxygen. That may not mean much when we’re sitting down and talking to each other, but when you do activities like go up stairs, go up an incline, you get winded sooner than you otherwise would because you’re not getting enough oxygen.
Falk: You’re shunting blood from the arterial tree to the venous tree much more rapidly. What happens in the brain? What are the symptoms in the brain?
Kasthuri: Stroke—hemorrhagic stroke is the dreaded complication from these brain AVMs.
How HHT is inherited
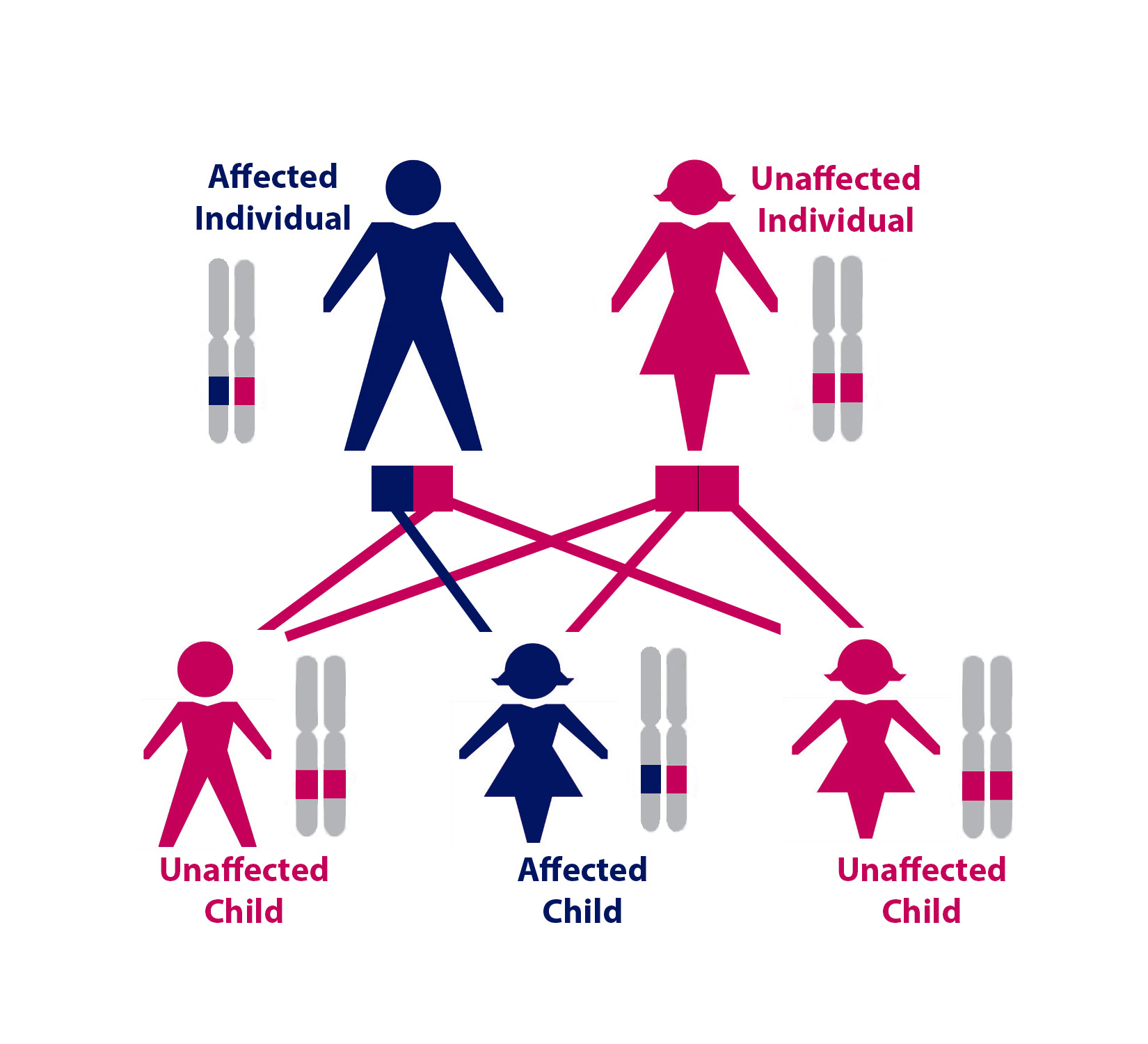
Falk: How is HHT inherited?
Kasthuri: It is inherited in an autosomal dominant fashion, meaning all you have to have is one affected gene to manifest the disease and to pass it on. Anybody who has HHT has a fifty percent chance of passing that on to their offspring.
Falk: How good is the genetic test for HHT at this point?
Kasthuri: The genetic test is good in the sense that if you have a pathogenic, or an HHT-associated mutation identified on genetic testing, that absolutely confirms the disease.
Falk: Is it one gene? Is it several genes?
Kasthuri: There are three genes that are known to be involved in HHT, and all of them are involved in various aspects of the same signaling pathway involving the lining of the blood vessel, the endothelium.
Falk: What are those genes?
Kasthuri: Endoglin, ACVRL1 or ALK-1, which are both part of the receptor complex on the surface of the endothelial cell for transforming growth factor beta, and SMAD4, which is downstream of this receptor complex. What’s interesting about SMAD4 is that it’s the same gene that causes juvenile polyposis. People who have HHT but have a SMAD4 mutation have a dual disorder—they have both juvenile polyposis and HHT.
Falk: Is one of those genes more frequently mutated than others?
Kasthuri: Eighty percent of HHT, we believe is explained by endoglin mutations, or ALK-1 mutations. Between the two of them, we think they’re pretty evenly spread, although there are pockets in the world where one is more common than the other. SMAD4 mutations are much less common—only three to five percent of patients with HHT will have it because of a SMAD4 mutation.
Falk: That leads me to eighty-three to eighty-four percent. What happened to the other seventeen percent?
Kasthuri: Excellent question—which is why I said genetic testing is good when you find the mutation, but fifteen percent of the time, even though somebody manifests clinically with all of the signs and symptoms of HHT, the genetic testing will be negative. In that setting, we have to make the diagnosis clinically.
HHT treatment
Falk: Right. If you have a diagnosis of HHT, what do you do? What are the treatments?
Kasthuri: There are a number of treatments, but no cure as yet. The way we treat HHT is to treat the symptoms related to the disorder—nosebleeds being the most common, we have to do a good job of treating nosebleeds. That involves simple measures that everybody who is affected can do at home, like using a humidifier overnight, like using topical moisturizers to the nose, to keep the mucus lining of the nose moist at all times. Depending on how severe they are, there are also surgical approaches and more and more medical treatments now that we use to control the development of these telangiectasias and the bleeding associated with it.
Falk: How about if you have shortness of breath because you have many arteriovenous malformations or AVMs in your lung? How do you handle that? Do you surgically go in, or radiologically go in and plug them up?
Kasthuri: Right, we go in primarily radiologically. In addition to treating the nosebleeds and the related complication from nosebleeds—which is anemia—up to fifty percent of people with HHT will develop iron deficiency anemia because of that, because it is ongoing bleeding.
In addition to that, there are guidelines as to how to look for or screen AVMs in the brain and the lungs and then to fix them if they meet certain criteria. The best way to pick up a lung AVM is to do a contrast echocardiogram, what we call a bubble echocardiogram. If that suggests that there is a shunt in the lungs, then we do a CT scan, look for these AVMs, and then if present and meet criteria where we can go fix it, we fix it with the help of interventional radiology. The radiologist goes in through the groin, just like an angiogram for the heart, and embolizes the pulmonary AVMs.
Falk: What’s the life expectancy, then, for somebody with HHT?
Kasthuri: We believe if all of the symptoms are treated and the AVMs are screened for, and fixed appropriately, a person with HHT should have a lifetime that is not much different from anybody else. If that is not done, then complications from these AVMs, or severe persistent anemia, could affect the life expectancy of a patient with HHT.
Falk: You said there are medical therapies on the horizon? What are those?
Kasthuri: The latest advance in HHT is the use of anti-angiogenic approaches to treat HHT, where we can use medications that are now approved primarily in the world of oncology to treat cancer as an adjunct to chemotherapy, and these drugs are targeted at the development of blood vessels, where they prevent the development of new blood vessels, which is something we can then exploit in a disorder where the problem is primarily development of abnormal new blood vessels.
HHT Centers of Excellence & Cure HHT
Falk: Fascinating. A patient with HHT, then, really needs an organization that specializes in taking care of these patients. It’s a multidisciplinary approach. What does it mean to be a Center of Excellence, an HHT Center of Excellence?
Kasthuri: HHT Centers of Excellence is a concept that was created in the early 90’s, primarily driven by a patient advocacy group that came together. It used to be called HHT Foundation International, now rebranded as Cure HHT, and they partnered with interested groups of physicians around the country to form centers where they provided all of the necessary components that you would need to provide one-stop care for HHT. That would involve a medical director who takes care of appropriate screening, an interventional radiologist who has expertise in embolizing these AVMs, a genetic counselor so patients and families can be educated about HHT, an ENT provider who has expertise in how best to take care of these nasal telangiectasias that cause bleeding, as well as less frequent complications of HHT such as pulmonary hypertension, high-output heart failure as a complication of liver AVMs. The idea is to bring all of this expertise together in one spot.
Falk: UNC has a Center for Excellence in HHT.
Kasthuri: Yes, the UNC HHT Center for Excellence was started in 2011.
Falk: How would you tell somebody who is not being seen in a center, who is just being diagnosed, where would you have them look to find more information about HHT?
Kasthuri: I would suggest people look at the Cure HHT website, it is CureHHT.org. It is a fantastic resource for patients and family members, where there is a lot of patient education material there. In addition, also a directory of current HHT Centers of Excellence so they can also guide patients to the closest HHT center where they could seek further management.
Challenges with awareness and access to care
Falk: What then are the challenges that the HHT community faces?
Kasthuri: I think the biggest challenge in the HHT community now would be awareness. The best data we have suggest that only about two out of ten people with HHT know what they have.
Falk: That’s a terribly low number.
Kasthuri: Yes, it is, so there’s a long way to go in terms of raising awareness, so patients understand what they have. A big part of this is also educating providers. Even if a patient does the right thing, goes to a physician and says, “I’ve got all these problems,”if the physician cannot make the diagnosis of HHT, then we’re going in circles. So, awareness, both providers and patients, is one big challenge.
The second is access to care. Even if you have HHT, there are only twenty-five HHT Centers of Excellence in our country right now, and not all twenty-five of them are in an individual state. There are three centers in California, and there are a number of states without a center. In today’s world, and the way things function with insurance, patients may not be able to get to an HHT Center, so access to care is another big problem.
Falk: What’s the way to answer those to issues, awareness and access?
Kasthuri: I will answer the second question first. In terms of access to care—and this is something that we recently are working on with the CDC and have a grant to work on. There is a very similar disease to HHT, which is hemophilia. Hemophilia has hemophilia treatment centers that are designated comprehensive models of multidisciplinary care. There is at least one hemophilia center in every state.
What we are now working on, is to see if we can educate the hemophilia center team to take care of HHT. We are conducting a pilot study right now. If that pans out, then that would be a quick solution to have HHT expertise in every state. That is a reasonably quick answer to try to address the access question. The awareness question is a more challenging one.
Falk: More podcasts.
Kasthuri: More podcasts, yes, indeed. Also, there are regional conferences. As we get more HHT centers and they do work in their community to educate and get the word out, that’s a way to increase awareness.
Falk: Raj Kasthuri, thank you so much for spending time with us today.
Kasthuri: Thank you.
Falk: Thanks so much to our listeners for tuning in. Next time, we will be talking to Dr. Anil Gehi about a genetic disease that affects the heart – known as the Long QT Syndrome. You can subscribe to the Chair’s Corner on iTunes, SoundCloud, or like us on FaceBook. Thanks so much for listening.
Visit these sites for more information:
// var audio; var playlist; var tracks; var current; init(); function init(){ current = 0; audio = $(‘audio’); playlist = $(‘#playlist’); tracks = playlist.find(‘li a’); len = tracks.length – 1; audio[0].volume = .90; playlist.find(‘a’).click(function(e){ e.preventDefault(); link = $(this); current = link.parent().index(); run(link, audio[0]); }); audio[0].addEventListener(‘ended’,function(e){ current++; if(current == len){ current = 0; link = playlist.find(‘a’)[0]; }else{ link = playlist.find(‘a’)[current]; } /* run($(link),audio[0]); stops from going to next track */ }); } function run(link, player){ player.src = link.attr(‘href’); par = link.parent(); par.addClass(‘active’).siblings().removeClass(‘active’); audio[0].load(); audio[0].play(); }