What is Long QT syndrome? Dr. Anil Gehi describes this genetic condition, the different types of Long QT, and the treatments. Dr. Gehi is an Associate Professor of Medicine in the Division of Cardiology and is Director of Clinical Cardiac Electrophysiology lab at UNC.

“If the QT interval is prolonged, patients can be at risk for ventricular rhythm disturbances… Instead of just being reset and activated again…it can on its own go into an abnormal rhythm. The lower chambers of the heart basically go haywire for a few seconds. They beat out of control very rapidly and that can lead to fainting spells and can lead to cardiac arrest and sudden death.”
– Dr. Anil Gehi
Ron Falk, MD: Hello, and welcome to the Chair’s Corner from the Department of Medicine at the University of North Carolina.
This is our series where we discuss different genetic diseases with physicians who treat patients with these conditions. Today, we will talk about something called the Long QT syndrome.
We welcome Dr. Anil Gehi, who is an Associate Professor of Medicine in our Division of Cardiology. Dr. Gehi is also Director of Clinical Cardiac Electrophysiology lab at UNC. Welcome, Dr. Gehi.
Anil Gehi, MD: Thank you. Thanks for having me.
The heart’s electrical system & long QT intervals
Falk: What on earth is Long QT? What does that mean?
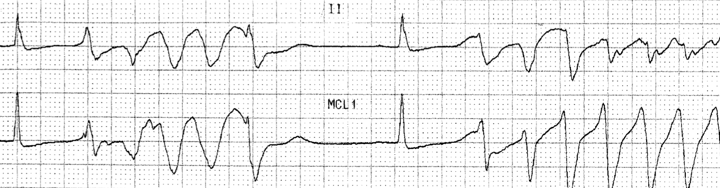
Gehi: Long QT syndrome is an electrical disorder of the heart. As you know, everybody’s heart has an electrical system that regulates the pace of the heartbeat. It slows down when you’re resting, it speeds up when you’re exercising. There are a lot of disorders of the electrical system, and one of those disorders is called Long QT syndrome. It’s characterized by a long QT interval, which is a thing we can measure on somebody’s electrocardiogram, which is basically a snapshot of the heart’s electrical system.
Falk: When you think of the electrical system of the heart—in so many ways the heart is a muscle that has blood vessels that supply the muscle, and when one has a heart attack, the blood supply to that muscle gets altered or stopped. In addition to those blood vessels, there are electrical fibers that tell the heart to beat in a coordinated fashion. How do you measure those electrical currents?
Gehi: This is an interesting problem. There is an electrical system of the heart that you can’t see visually—if you were to take a picture of somebody’s heart, you wouldn’t be able to see the electrical system. We look at it by using an electrocardiogram.
Falk: AN EKG.
Gehi: An EKG basically is a snapshot of somebody’s electrical system. What we do to do that is we put electrodes on the surface of the person and measure the electrical activity that’s happening in the heart. That’s our snapshot of the electrical system.
Falk: You can also measure somebody’s electrical system sometimes over days, not just a snapshot. You can put an EKG device on somebody and have them walk around.
Gehi: That’s correct. We do ambulatory monitoring, so we’ll have somebody wear an EKG that they can walk around with, and we can see rhythm disorders that might happen intermittently.
Falk: Sometimes people have very, very fast heart rates that are abnormal and are dangerous.
Gehi: Exactly. There are many, many different abnormalities of the heart. My whole career is devoted to that. Long QT syndrome is one of them, and it’s one that is particularly worrisome because it can lead to sudden death.
Falk: On an EKG, you’re looking for certain types of waves or forms, and there are various complexes that you look at. Can you just name those for us so our listeners understand?
Gehi: Certainly. The different complexes have letters associated with them. There’s the P wave, the QRS complex, the T wave. Those correlate with different phases of the electrical activity of the heart. Each time the heart beats, there’s electrical activity that initiates that heartbeat, and that electrical activity is depicted by those different phases that we see on the EKG. The QT itself is actually the resetting part of that electrical activity. When the electrical system says to initiate a heartbeat, there is this process of activating the myocardial cells, or the heart cells. That’s depicted by the QRS complex on the EKG. Then after it’s activated, it needs to be reset. That resetting process is depicted by the QT interval.
There’s an automated read on the EKG that will measure the QT interval that’s basically telling us how long it takes for that resetting to happen in the muscle cells.
Falk: The resetting should happen in a predictable fashion each and every time.
Gehi: That’s right. Each time it’s reset, it happens in a predictable fashion so that it’s ready for the next activation.
Falk: If the QT interval, the reset time in other words, gets prolonged, what happens?
Gehi: There are problems of the electrical system that are characterized by a prolonged QT interval. If the QT interval is prolonged, patients can be at risk for ventricular rhythm disturbances. That means, basically an electrical disorder of the lower chambers of the heart. Instead of just being reset and activated again when your natural pacemaker says to be active again, it can on its own go into an abnormal rhythm. The lower chambers of the heart basically go haywire for a few seconds. They beat out of control very rapidly and that can lead to fainting spells and can lead to cardiac arrest and sudden death.
Falk: Unfortunately, that happens in young people as well as old people, but for different reasons.
Gehi: That’s right. Long QT syndrome is one of those disorders that people are born with, so it will affect young people and young adults very often.
Inheritance pattern of Long QT & testing
Falk: How is it inherited?
Gehi: It’s inherited in an autosomal dominant fashion, meaning that if someone has it, there’s a fifty percent chance of them passing it on to their children.
Falk: Which is really a scary thought there—you’re a parent and you might not even know that you have it, and pass along a gene that could end up causing your child’s death.
Gehi: That’s right. What we do, then, is when we find it in somebody—“the proband,” then we will make sure to screen family members for that same syndrome. We can screen by EKG and look for the long QT. Then, if the patient has a genetic abnormality identified, we can test for that specific genetic abnormality.
Falk: What are those genetic abnormalities?
Gehi: There are a whole slew of them. We now have about thirteen different genes that have been implicated with Long QT syndrome. There are three of them that are the most common that account for about ninety percent of the Long QT syndrome patients we’ve identified. Then there are a whole host of mutations in those genes.
Falk: What are those genes?
Gehi: They basically are the genes that are responsible for the creation of ion channels. The ion channels are those channels on the muscle cells that allow for the flow of ions in and out of cells and basically create the electrical activity. So, if there are mutations in the genes responsible for the creation of the ion channels, then you could end up with the Long QT syndrome.
Falk: If you suspect, then, a patient having Long QT syndrome, how do you test them? Do you test them with EKG, with genetic test, do you do both?
Gehi: We do both. Generally, we’ll be suspicious of Long QT. First of all, if someone has a long QT on their EKG, particularly if they have symptoms associated with Long QT syndrome, such as fainting spells, or if they had had a cardiac arrest and had been resuscitated, then we will be suspicious of it and we will give them the diagnosis if they have some of the features. The length of their QT is part of the diagnosis, the symptoms are part of the diagnosis, if they have a family history, that’s also part of the diagnosis. Then we can further classify the type of Long QT syndrome that they have by doing genetic testing.
Different types of Long QT
Falk: There are different kinds of Long QT and there are numbers associated with them.
Gehi: That’s right.
Falk: Tell us a little about them.
Gehi: There are about thirteen of them that have been described, but the most common ones are type 1, type 2, type 3. It’s quite interesting in that they have very specific clinical manifestations. For example, type 1, which is the most common, has the manifestation of having events during exercise, the classic one is swimming. You hear about a person who has a near-drowning episode, or a person who faints while exercising. That’s a big red flag for us and one of the things we would look for is Long QT type 1. Their QT interval actually will lengthen as they exercise, and they are prone to having these ventricular arrhythmic events during exercise.
Falk: Why swimming?
Gehi: I don’t know why it’s swimming, it’s very interesting, but that’s been the characteristic type of exercise. Type two also can happen during exercise, but less likely. It’s more common to happen during emotional stimuli—again, I don’t know why that is. The classic is a sudden auditory stimulus like an alarm clock. An alarm clock goes off, and suddenly they have an episode. One of the things we tell people with Long QT type 2, is “Get rid of your alarm clocks.”
Falk: That’s wonderful. You can sleep in!
Gehi: That’s right! The type 3, which is the third of the most common ones, is the most lethal, because events happen during sleep. They just don’t wake up. We don’t know about the patient, they have an episode during sleep. That’s one of the more lethal ones, so that’s one of the features of being high risk. If someone has Long QT type 3, we consider them at high risk.
Falk: Wow. The whole concept of not being able to handle an alarm clock or swim is pretty remarkable.
Falk: One other question about the different types. Do you pass along exactly that type from generation to generation?
Gehi: Yes, basically. Once you have a mutation identified, there’s a fifty percent chance of passing that same one on to your child.
Acquired Long QT syndrome
Falk: There are non-inherited forms of Long QT. There are many types of drugs or pharmaceutical agents that also can prolong the QT interval—some common drugs, actually.
Gehi: That’s correct. We actually divide Long QT syndrome into what we call inherited Long QT syndrome and acquired Long QT syndrome. Acquired Long QT syndrome is really mostly due to those medications that can cause QT prolongation. There are many antibiotics, anti-seizure medicines, for example, that can cause your QT to lengthen—a whole host of medications can cause acquired Long QT. Also, electrolyte abnormalities—patients, for example, who are depleted of potassium or magnesium can have a lengthening QT.
We put those patients into what we call acquired Long QT, and that’s important to distinguish, because those are potentially treatable, and not something that necessarily will be passed onto their children.
Falk: Eat your fruits, vegetables, and almonds for your magnesium, at least you’ll take care of those electrolytes.
Gehi: That’s right.
Falk: If it’s an acquired process, that’s really treatable by getting rid of the underlying disorder—underlying medication, underlying electrolyte disorder—that’s relatively easier, I suppose.
Gehi: Generally. I will say that there is probably a little bit of overlap. For example, there are patients who take a medication that lengthens their QT, but they may in fact have a milder form of inherited Long QT underlying that is unmasked by the drug. There may be some overlap, but for the most part, yes, if they have acquired Long QT, and stop the medication, correct the electrolyte abnormalities, and then they usually won’t have to deal with any consequences.
Long QT treatments
Falk: How do you treat inherited forms of Long QT?
Gehi: The treatment depends on the severity, so what we’ll do initially when we have a patient who is suspected for Long QT, is we will risk stratify them, and that risk stratification is based on how long their QT interval is. For example, if somebody’s QT interval is very, very long, they have a higher risk.
Falk: How long?
Gehi: A long QT is by definition, more than 460 or so. Women actually have a little bit longer QT than men, so our cutoffs are a little higher in women, but if it’s above 460, that’s considered long. It’s very long when it’s above 500. If somebody has a very long QT, they are at higher risk of events. If somebody has had a prior event—a fainting spell, for example, or a resuscitated cardiac arrest, they are at very high risk. So, we’ll go through this process of risk stratifying them.
Genetic testing can also be part of that. Certain genetic abnormalities or certain genes that are affected are at higher risk than others. Once we have gone through that risk stratification, that will help determine what the therapies are. Those therapies could be something as simple as, “This is mild—you just need to avoid taking medications that prolong the QT,” or if it’s a higher risk, sometimes we’ll treat patients with a beta blocker medication that can help prevent episodes of fainting and cardiac arrest.
The most severe ones, for example people who have had a cardiac arrest and survived, or have a very long QT and maybe have one of the worsened genetic mutations, will end up needing a defibrillator. A defibrillator is a device that will protect them from a cardiac arrest.
Falk: And it’s implanted in the chest with wires or leads that go right into the heart.
Gehi: That’s right, it’s basically what we call “a paramedic in your chest”—it watches your heart. If you have one of these bad, lethal rhythms, it will protect you and resuscitate you.
Falk: For the most part, people with Long QT syndrome, if they understand what is wrong, are willing to have a defibrillator if necessary.
Gehi: That’s right. If you have a severe abnormality, and you, for example, have been resuscitated from a cardiac arrest, we would say you are at high risk for this happening again, and we would recommend a defibrillator, and most patients would be willing to do that.
Falk: If you have a family member who has not had a cardiac arrest, and by a screening process discover that another sibling has a very long QT, would you suggest that they get a defibrillator?
Gehi: That’s a tough question. It’s pretty rare that we would put a defibrillator in a patient who has never had a symptom. One thing—to take a step back and explain—even though it is inherited, there is a fifty percent chance of getting the problem if your parent has it. There is what we call “variable penetrance,” meaning that you could get the genetic abnormality but it not be as severe. We will always look for the genetic abnormality but correlate that with symptoms and clinical manifestations. So, if a patient has the clinical manifestation and they are high risk, then yes, sometimes we will put a defibrillator in, but most of the time, we’ll use the defibrillator only on those patients who have had symptoms.
Falk: There are risks of having a defibrillator.
Gehi: Absolutely. Having a device implanted in your chest for a long time has its risks, and when we’re talking about young adults here, that’s a long, long time to have a defibrillator. Defibrillators can have problems with their leads, they will need battery changes periodically, so there are major consequences to having a defibrillator. So, we only want to put them in people who absolutely need it.
Falk: If you have received treatment of any of the kinds you’ve described, what’s the outlook of somebody with Long QT?
Gehi: It’s actually very good. We have treatments for it, they are very effective. Beta blockers are very effective medicines, particularly for certain forms of Long QT. There is the most common one, which is Long QT type 1, which is the one that’s characterized by having episodes during exercise. That one is very, very treatable with beta blockers. So, it’s actually quite rare that you need to use a defibrillator in those patients. As long as the patient takes the beta blocker, then generally they can be very well protected and have a normal life.
More information on Long QT
Falk: Where would you tell someone who has Long QT or a family member to find additional information?
Gehi: A couple of things. First off, someone who has Long QT, it’s very important that they avoid QT-prolonging drugs. There’s a nice website called QTdrugs.org that has a running list of those medications that we always tell patients who have Long QT to go anytime they’re starting a new medication. Another place they can go, there’s an organization called Sudden Arrhythmic Death Syndrome Foundation. They have a nice website—SADS.org where there’s a lot of patient-appropriate information.
Falk: Thank you so much, Dr. Gehi, for providing this really fascinating discussion.
Gehi: Thank you.
Falk: Thanks so much to our listeners for tuning in. Next time, we will be talking with Dr. Sid Barritt about hemochromatosis. You can subscribe to the Chair’s Corner on iTunes, SoundCloud, or like us on FaceBook.
Visit these sites for more information:
// var audio; var playlist; var tracks; var current; init(); function init(){ current = 0; audio = $(‘audio’); playlist = $(‘#playlist’); tracks = playlist.find(‘li a’); len = tracks.length – 1; audio[0].volume = .90; playlist.find(‘a’).click(function(e){ e.preventDefault(); link = $(this); current = link.parent().index(); run(link, audio[0]); }); audio[0].addEventListener(‘ended’,function(e){ current++; if(current == len){ current = 0; link = playlist.find(‘a’)[0]; }else{ link = playlist.find(‘a’)[current]; } /* run($(link),audio[0]); stops from going to next track */ }); } function run(link, player){ player.src = link.attr(‘href’); par = link.parent(); par.addClass(‘active’).siblings().removeClass(‘active’); audio[0].load(); audio[0].play(); }