A Fighter All Her Life, Surviving an Unsurvivable Condition
Finding the diagnosis
Acid reflux. That’s what doctors initially thought Helen Nance was suffering from. Her primary doctor listened to her complaints of nausea on August 24th and did an ultrasound. The tests were inconclusive, so they set up an endoscopy for the following day. That way, doctors could use a camera to look down her esophagus to see what was going on. Unfortunately, for Helen, she never made it to that appointment.
Instead, that evening she headed home with her daughter June for some dinner and rest. “We ate, and then I sat on the couch,” recalls Helen. “I hadn’t been sitting there long when I told her (June) that I didn’t feel good. I felt like I had to throw up so I went to the bathroom. The first thing I did, I knew I was going to throw up, so I got on my knees in front of the toilet. I threw up nothing but blood. That’s the only thing I experienced. I don’t remember anything after that.”

June rushed Helen to the Emergency Department at Southeast Regional Medical Center in Lumberton. Doctors ran a gamut of tests on her, including X-rays and a CT scan. When the tests came back, doctors weren’t sure what was happening, but they knew her situation was critical. UNC airlifted Helen to UNC Hospitals in Chapel Hill. It was there that Helen and June met Gita Mody, MD, MPH, Director of Thoracic Surgical Oncology and Assistant Professor of Surgery at UNC.
Receiving Care At UNC
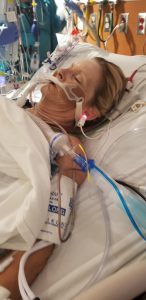 Dr. Mody explained to Helen and June what happened. It turned out that Helen had a descending thoracic aortic aneurysm. The aorta is the largest blood vessel in the human body. It leaves the heart and forms an arch. The arch’s downward portion, called the descending aorta, is connected to a network of arteries that supply most of the body with oxygen-rich blood. An aneurysm is a bulge that forms in the wall of an artery. It happens when the artery wall weakens. Aneurysms are dangerous because they can rupture and cause massive internal bleeding.
Dr. Mody explained to Helen and June what happened. It turned out that Helen had a descending thoracic aortic aneurysm. The aorta is the largest blood vessel in the human body. It leaves the heart and forms an arch. The arch’s downward portion, called the descending aorta, is connected to a network of arteries that supply most of the body with oxygen-rich blood. An aneurysm is a bulge that forms in the wall of an artery. It happens when the artery wall weakens. Aneurysms are dangerous because they can rupture and cause massive internal bleeding.
That is precisely what happened to Helen. Not only did her aneurysm rupture, but it also tore into the esophagus, causing an aortaesophageal fistula. Blood was filling up her abdomen quickly, forcing doctors to rush Helen into the operating room.
“I was on call when they flew Helen to the hospital. She went straight to the ICU due to her critical condition. Thankfully, she had stabilized briefly.,” explains Dr. Mody. “While she may not remember the experience, she was awake, alert, and came to tears during our conversation. I introduced her to Dr. Ezequiel Parodi, Vascular Surgeon and Associate Professor. We needed to close the hole in her aorta before opening her chest and tackling the esophagus part.”

As the first step in the operation, Dr. Parodi performed a thoracic endovascular aortic repair (TEVAR). TEVAR is a minimally invasive surgery. That means it’s performed with a small incision. With TEVAR, a device called a stent-graft is used to reinforce the aneurysm. A stent-graft is a metal tube covered in fabric. It redirects blood flow to uninjured sections above and below the ruptured portion of the aorta.
“This was one of my first cases at UNC,” explains Dr. Parodi. “Ruptured aortic aneurysms have up to a 90% mortality. Most series show that even when the patient makes it to the hospital and has a TEVAR the morality can reach 20-30%. That does not include the Mortality of the aortic esophageal fistula. I saw this patient in the clinic recently and she has made a remarkable recovery. Her aortic repair is intact and she is enjoying a good quality of life. This was a great team effort from UNC surgery.
The surgery was successful, but during the procedure Helen became unstable, forcing the doctors to leave her intubated until her heart could stabilize.
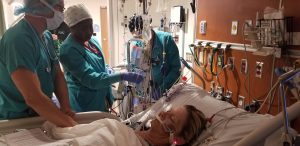 The following day, Helen was stable enough to go back into the operating room. Dr. Mody performed an esophagectomy, opening her chest and removing her esophagus with plans to reconstruct it at a later date when Helen recovered. Her esophagus was not connected to her stomach anymore but rather was sutured to her neck. The surgery was successful but left her with a spit fistula, a bag attached to her neck that would allow for proper drainage of fluids.
The following day, Helen was stable enough to go back into the operating room. Dr. Mody performed an esophagectomy, opening her chest and removing her esophagus with plans to reconstruct it at a later date when Helen recovered. Her esophagus was not connected to her stomach anymore but rather was sutured to her neck. The surgery was successful but left her with a spit fistula, a bag attached to her neck that would allow for proper drainage of fluids.
“When they finished with me, went as far as they could with me here, they sent me to Fayetteville,” explains Helen. “It’s a part of Cape Fear called Highsmith-Reiney Hospital, a specialty hospital. I had my rehab there for three months, and I stayed there from September until December 11th. December 12th was the day that I had surgery at UNC for my esophagus.”
Improving Quality of Life after a miraculous recovery

The removal of her esophagus was just the first step for Helen. Her final surgery was performed by Dr. Mody and Dr. Michael Meyers, Professor of Surgery, Surgical Oncologist, and an expert in gastrointestinal operations. As a team, Drs. Mody and Meyers performed a substernal gastric pull-up. The stomach is used to replace the missing esophagus and needs to be brought up from the abdomen into the chest and reconnected in the neck. She came through the long surgery well. Now she needed to heal the new connections or new esophagus.
“Fortunately her stomach was healthy and we could use this to reconstruct her esophagus,” explains Dr. Meyers “We will sometimes use the colon instead, but when possible the stomach usually functions better after she has healed from surgery”
A Christmas Gift
On December 24th, Helen was released from UNC into the care of her daughter June. They arrived home in Lumberton, NC, at 2 am and were able to enjoy Christmas at home with their family. She was on the road to recovery. While her new esophagus healed, Helen utilized a feeding tube until it was removed at her clinical visit on February 25th. She was able to enjoy Christmas dinner.
Throughout the entire process, Dr. Mody remained watching over Helen’s recovery. During her follow-up visits, Helen, June, and Dr. Mody would discuss how Helen was feeling and the next steps in her care.
“Helen is a spitfire of a woman,” says Dr. Mody. “She has the heart of a fighter, which has helped her to weather every challenge during this difficult experience. It took a team of doctors across multiple disciplines, along with nurses, staff, and caretakers to help her recover, but it was Helen herself that did the most important work. She fought to survive.”
Family First
 Throughout the entire experience, Helen stayed positive. When given the all-clear to get back to the regular activities of life, her club of bowling ladies welcomed her with open arms. She started to take part in the things she missed while recovering. Most importantly, though, she is grateful for the love and support of family and friends, especially one person who hardly left her side. “I don’t know what I would have done without June,” Helen says, “because she was there for me from the get-go. There’s no way to explain it because she has been there for me for everything. She was worse than my mom would have been getting after me about doing something I shouldn’t do.”
Throughout the entire experience, Helen stayed positive. When given the all-clear to get back to the regular activities of life, her club of bowling ladies welcomed her with open arms. She started to take part in the things she missed while recovering. Most importantly, though, she is grateful for the love and support of family and friends, especially one person who hardly left her side. “I don’t know what I would have done without June,” Helen says, “because she was there for me from the get-go. There’s no way to explain it because she has been there for me for everything. She was worse than my mom would have been getting after me about doing something I shouldn’t do.”
 As her caregiver, June stayed by Helen’s side throughout the long hours of surgery and the long days in the hospital and rehab. After leaving the hospital Helen stayed with June until Dr. Mody gave her the approval to head back to her own home. She was there for every decision, word of advice, and piece of information that doctors had to impart. “I was here almost the whole time,” June says. “I tried to go home on the weekends. Even at the hospital in Fayetteville, I’d be there except for on the weekends. I guess I would be considered a caregiver but I was treated no less than her (Helen). Everyone made me feel welcome and comfortable.”
As her caregiver, June stayed by Helen’s side throughout the long hours of surgery and the long days in the hospital and rehab. After leaving the hospital Helen stayed with June until Dr. Mody gave her the approval to head back to her own home. She was there for every decision, word of advice, and piece of information that doctors had to impart. “I was here almost the whole time,” June says. “I tried to go home on the weekends. Even at the hospital in Fayetteville, I’d be there except for on the weekends. I guess I would be considered a caregiver but I was treated no less than her (Helen). Everyone made me feel welcome and comfortable.”
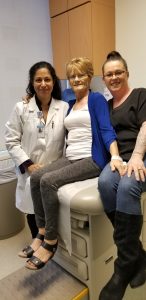 Helen thinks back to her entire medical journey, “I have to say UNC Hospital, the nurses, all the staff, doctors, everybody was amazing. They have been wonderful. Especially Dr. Mody, she is special and has been an incredible doctor. I’m also thankful for my rehab staff at the Hospital in Fayetteville. I love those people. They were so good to me. I thank God; he allowed me to live for some reason. I know people who have had the same thing happen and they did not make it. I thank God. He allowed me to live and allowed those doctors to put their hands on me, to guide their hands so that I could live to tell the story.”
Helen thinks back to her entire medical journey, “I have to say UNC Hospital, the nurses, all the staff, doctors, everybody was amazing. They have been wonderful. Especially Dr. Mody, she is special and has been an incredible doctor. I’m also thankful for my rehab staff at the Hospital in Fayetteville. I love those people. They were so good to me. I thank God; he allowed me to live for some reason. I know people who have had the same thing happen and they did not make it. I thank God. He allowed me to live and allowed those doctors to put their hands on me, to guide their hands so that I could live to tell the story.”