Advocating for His Health
 Standing outside in the fresh air, a crisp winter morning, looking at a clear blue sky and taking a long deep breath, feeling the cold air fill your lungs. It sounds simple, easy. However, for Ronald Campbell, there was a time when taking a breath, any breath was a struggle. Imagine having a hard time taking a shower, physically able to but just trying to wash, perform the most basic tasks, is a struggle because you can’t breathe. This was the stark reality for Ronald Campbell, a 45-year-old father of two living in Raleigh, North Carolina when his condition was at its worst.
Standing outside in the fresh air, a crisp winter morning, looking at a clear blue sky and taking a long deep breath, feeling the cold air fill your lungs. It sounds simple, easy. However, for Ronald Campbell, there was a time when taking a breath, any breath was a struggle. Imagine having a hard time taking a shower, physically able to but just trying to wash, perform the most basic tasks, is a struggle because you can’t breathe. This was the stark reality for Ronald Campbell, a 45-year-old father of two living in Raleigh, North Carolina when his condition was at its worst.
In late 2017 during his annual physical, Ronald mentioned to his primary care doctor that he was experiencing difficulty breathing during exercise and other strenuous activities. The physician prescribed a rescue inhaler and shuffled him out the door with a note to schedule his next checkup in a year.
In late May/early June of 2018, Ronald headed to WakeMed ER because he thought something was wrong with his heart. “I couldn’t catch my breath,” recalls Ronald. “My heart was racing, and it felt like someone was standing on my chest. After a stress test, the cardiologist told me that while my heart was fine, something was ‘going on with my lungs.’” After discharge, Ronald went back to his primary care and continued the cycle of non-care shuffled back and forth between doctors.
Over the next few years, Ronald would mention his lungs and his worsening breathing at every primary care and rheumatologist visit. He was told, “lose 5 pounds” or “tell your primary care,” etc. Finally, in June 2020 (in the midst of a global pandemic), he went back to the doctor and wouldn’t leave until he received a referral to a pulmonologist. He received the referral but couldn’t get an appointment for another month. As the summer passed, his condition worsened. Walking became more of a challenge, as did almost every other activity.
In late August, Ronald finally saw the pulmonologist, Dr. Hall, at UNC REX in Raleigh and Physician Assistant Stacey Roper. Everything changed. He immediately diagnosed him with interstitial lung disease. Per the American Lung Association, “Interstitial lung disease (ILD) is an umbrella term used for a large group of diseases that cause scarring (fibrosis) of the lungs. The scarring causes stiffness in the lungs, making it difficult to breathe and get oxygen to the bloodstream. Lung damage from ILDs is often irreversible and gets worse over time.” Dr. Hall referred him to a pulmonology specialist, Dr. Jason Lobo, the Kimberly H. Tsamoutales Distinguished Term Professor of Medicine, Pulmonary Diseases and Critical Care Medicine, and the Medical Director of Pulmonary Transplant and Interstitial Lung Disease at UNC in Chapel Hill.
At UNC, he received a pulmonary function test (PFT) that showed his lung function to be around 45% of a fully healthy lung. They performed blood oxygen saturation tests and determined that he needed to sleep with supplemental oxygen.
Dr. Lobo told Ronald he wished he had met him two years earlier. “While I shared his sentiment,” says Ronald, “I was elated to have someone listening to me finally. I felt like my doctors at REX, and Dr. Lobo was my medical advocate trying to help me feel better. Dr. Lobo informed me that transplantation was on the table, but he wanted to do everything to put that off as long as possible. He prescribed a whole mess of medications that had shown efficacy in the past, with the caveat that it didn’t work for everyone and that transplant might still need to happen. October turned to November, and there was little improvement to my condition. I met with him in late November, and he was displeased with the effectiveness of the medication.”
Road to Transplantation
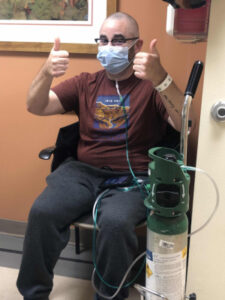 On December 7th, during his appointment with the pulmonologist, it was clear that Ronald’s condition was worsening. He went on 24-hour oxygen, and doctors started him on the road to lung transplantation. He had blood drawn for testing, a chest x-ray, and another PFT, which put his lung function at 26%. His lungs looked much like a cocoon, thick and fibrous. He had also to complete a 6-minute walk. “The point of this test is to show that you’re strong enough for surgery,” says Ronald. “I had to walk, with as much oxygen as I needed, 1000 feet in 6 minutes. If possible. Once they hooked me up to 27L of oxygen, I started. I was super proud to complete the test.”
On December 7th, during his appointment with the pulmonologist, it was clear that Ronald’s condition was worsening. He went on 24-hour oxygen, and doctors started him on the road to lung transplantation. He had blood drawn for testing, a chest x-ray, and another PFT, which put his lung function at 26%. His lungs looked much like a cocoon, thick and fibrous. He had also to complete a 6-minute walk. “The point of this test is to show that you’re strong enough for surgery,” says Ronald. “I had to walk, with as much oxygen as I needed, 1000 feet in 6 minutes. If possible. Once they hooked me up to 27L of oxygen, I started. I was super proud to complete the test.”
From there, he met with the nurse coordinator, other doctors and had a CT scan done. He also had virtual meetings with the social worker, nutritionist, psychologist, and financial person. While the testing and physician appointment process is usually spread out over a six to eight-week process, because of Ronald’s deteriorating condition, doctors accelerated the process for him to get him on the list for transplant as soon as possible.
Ronald started by first getting a heart catheterization, a procedure to examine how well his heart was functioning. Next up was a bone density scan, chest fluoroscopy, a CT scan of his abdomen and pelvis, and a check of his esophagus to see how his other organs worked. They checked his kidneys and performed multiple lung scans.

With each day, appointment, and test, Ronald got one day closer to transplantation. He met with the nurse coordinator, who helped walk him through the logistics and paperwork involved in surgery to replace a major organ. Next up was Ronald’s consultation with the thoracic surgeon, Dr. Benjamin Haithcock, Surgical Director of the UNC Lung Transplant Program.
“Dr. Haithcock was awesome,” says Ronald. “He is knowledgeable and has a great sense of humor that was good for putting me at ease. Dr. Haithcock described the surgery (comparing it to opening the hood of a car), the recovery, and the risks. I asked if he had any concerns about my specific case, given what he knew, and he said no. He said he was ready to rock.”
Some of the final steps for Ronald included a meeting with an infectious disease doctor. Because bacteria and other microbes come in and out of the lungs, doctors want to ensure that the patient is appropriately covered with antibiotics and that their immunizations are up to date. Doctors wish to confirm that no significant infectious disease issues are going into the operating room. Patients are immune-compromised once the surgery is complete and can pick up bacteria or infections, so infectious disease doctors are actively involved with all transplant patients.
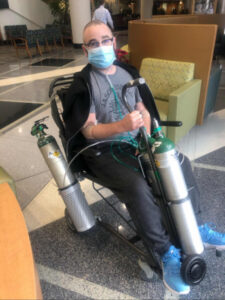 Finally, he got to the last step in his process, an appointment at the pulmonary rehab clinic that established whether he was fit enough for the surgery. In most cases, this is the first step in the transplant journey because many patients cannot meet the minimum requirements and are then put on a plan to get them ready for the surgery. Due to Ronald’s accelerated case, this step came last.
Finally, he got to the last step in his process, an appointment at the pulmonary rehab clinic that established whether he was fit enough for the surgery. In most cases, this is the first step in the transplant journey because many patients cannot meet the minimum requirements and are then put on a plan to get them ready for the surgery. Due to Ronald’s accelerated case, this step came last.
“Some years ago, I was on a small albatross (charter plane) flying from Havana to Miami,” remembers Ronald. “The two people in the front, I assumed to be the pilots, looked a bit sketchy. As we headed to the runway, they stopped the plane, opened the windows, and got some instructions. The flight was a non-event, but one thing about an albatross is that they are not good at landing. These two landed the plane, skidded sideways into a stop, looked at each other, and then high-fived. I took that to mean that this was their first successful landing.”
The therapist hooked him up to 30L of oxygen, and he was off. Test 1 was to stand up and sit down in a chair as many times as he could in 30 seconds without using the armrest. The goal is 12. He made 19-crushed it! Next, he had to stand from a chair, walk a short distance, and sit back down. The goal was 12 seconds. He did it in 7. Last- walk 1000 feet in 6 minutes. Off he went. He started strong at a record-breaking pace, but the therapist had to replace one of his oxygen tanks with one lap to go. The time didn’t stop! He looked down the hall, looked at the watch, saw seconds ticking by, and started to gauge when he’d have to run. He completed half of the last lap, saw that he had seconds to go, and he skidded to a stop in the chair at the end, 6 minutes on the dot. He high-fived the pulmonary therapist. The albatross had landed.
Dry Run
While the doctors and nurses were hopeful that Ronald would quickly get a new set of lungs, the process could take some time. The waiting can be challenging, especially during the pandemic, since a COVID diagnosis could derail all the hard work he had put in to get on the top of the transplant list. To stay safe, Ronald spent much of his time alone, solitary, in his room reading, watching television, and playing on his Nintendo Switch.
In early February, Ronald got the call. At 1 in the morning, the ringing of the phone sliced through the silence of his house. He answered it was the nurse coordinator who informed him it was time. Ronald and his wife Erin collected their stuff, hugged his two daughters goodbye, and made their way to the ER at UNC Health in Chapel Hill.
The surgery was scheduled for noon that day, so Ronald and his wife settled in to wait. Around 8 in the morning, the surgeon came in to see them and discuss the upcoming surgery. However, it was not Dr. Haithcock, the surgeon Ronald had initially met. Instead, Dr. Jason Long, Co-Director of the UNC Lung Cancer Screening Clinic, spoke with Ronald about the potential lungs and let him know that they noticed an area causing some concern on the lungs, but they can’t say for sure until they were removed from the donor.
Around noon, Ronald was transferred to the pre-op area. He met with the anesthesiologist and signed more consent forms. He got into the hospital gown, put on the hairnet, and waited, laying in the bed, looking at the doors to the operating area. He was inches away from an experience that would change his whole life. He called his daughters to say he loved them, and the surgeon walked in. He told Ronald and Erin that a spot on the lungs showed up on the CT scan and was confirmed with a visual inspection. Dr. Long wanted to turn them down; he wanted to give Ronald a perfect set of lungs.
“I cried,” recalls Ronald. “He is the expert, so we trusted his judgment. Minutes from surgery and inches from the room, everything came crashing down. Everything. I was so damn close. I spent the entire morning getting my head right. I was scared, excited, and anxious; you name it, I felt it. I had doubts. The staff tried hard to manage expectations, but I was ready once I got to pre-op, and I took off my clothes. I was ready for whatever was on the other side of that door-physically and metaphorically. Then it was all gone. I have never experienced the swing of emotions that I experienced on that day. I was devastated; it was gut-wrenching and crushing.”
It would be another couple of weeks before Ronald finally got the green light, and his surgery was a go.
Surgery and Recovery
On Sunday, February 21st, 2021, he got the call. At 6:30 in the morning, the first call that he excitedly answered was from AT&T, which wanted to lower his rates. On that high note, Ronald’s Sunday was off to an exciting start. However, 12 hours later, he got the call from the nurse navigator telling him it was time. Yet again, Ronald and Erin hugged the girls, packed up their stuff, and headed to UNC Health in Chapel Hill.
They settled into an emergency room-cardiac care bay to wait until the following day. Around 5 pm, he was wheeled to pre-op. Again, he got into the hospital gown, put the hairnet on, and waited. He looked at the surgery doors wondering if it was going to happen.
Ronald went into surgery at 6 pm on Monday, February 22nd, 2021.
“In the operating room, we take care to remove the patient’s native lungs safely and appropriately,” explains Dr. Haithcock. “Our team makes sure the patient is stable, that the connections are appropriate, and there is no significant bleeding after surgery. We also make sure the heart is doing well, and of course, the new lungs are getting the blood and air they need, moving up and down the way they should, with no compromise of the new organs. We know immediately if they are working, and for Ronald, the lungs looked wonderful.”
Immediately after surgery, patients are on a ventilator. As soon as the surgeons close the surgical incision, they get the patient off the ventilator. Typically, the ventilator is removed around 24 hours after the operation. Doctors want to get the patient up and walking as soon as possible after surgery.
“Patients feel like they’ve been hit by a truck and then the truck backs over them again.,” describes Dr. Haithcock. “Our goal is to get people up and moving around quickly to get their new lungs working. We do take great effort to make sure their pain is tolerable; our anesthesia does a great job with this.”
The Next Step…Recovery
 When Ronald’s breathing tube was removed, he was asked, “How does it feel?” “What?” Ronald said. “’ You’re breathing on your own.’ That is how I learned that I was using new lungs. I wasn’t expecting to have to teach myself how to breathe again, but I did. I had to constantly remind myself that I could take a deep breath again.”
When Ronald’s breathing tube was removed, he was asked, “How does it feel?” “What?” Ronald said. “’ You’re breathing on your own.’ That is how I learned that I was using new lungs. I wasn’t expecting to have to teach myself how to breathe again, but I did. I had to constantly remind myself that I could take a deep breath again.”
Over the next few days in the hospital, Ronald was monitored. Tubes were removed, and eventually, Ronald was untethered from everything. It was the first time in months he could move freely, unencumbered by breathing apparatus.
“Once Erin left in the evenings, I had lots of time to think,” says Ronald. “Honestly, I was having trouble with that part. My emotions ran through every possible iteration human emotion could go. I was grateful but scared. I was hopeful but anxious. I looked forward to the future but had a hard time with the present. I was overwhelmed. People would ask me, ’how does it feel?’ My answer was, ‘I don’t know.’ It felt nice to be able to take a deep breath, but every time I looked down at my chest, I would see the scars. I looked forward to a day they healed, and it didn’t hurt anymore. Recovery, mentally more than physical, was by far, without a doubt, the hardest thing I ever had to do.”
Over the next few months, Ronald began to heal. He went to every doctor, physical therapy, and medical provider appointment. Each day brought him closer to recovery. Closer to important moments in his life and the lives of his family.
When the year began for the Campbell family, everything seemed to be in flux. His daughters Emma and Rachel had to remotely navigate their senior and freshman years while watching their father’s health deteriorate. “It felt like every time there was a glimmer of optimism,” says Ronald, “it would be snatched from them at the last second. As 2021 began, it looked like a continuation of 2020. Then things began to move. I did all of my pre-transplant testing to be listed, there was talk of a return to school, and the vaccine was becoming a reality. Heck, they even said that there would be football and that the band would be there in some form. With that announcement, the date of March 26th loomed large. This would be senior night. The night Erin and I would walk Emma across the field to recognize her for her time in the band. Then on February 21st, I got the call. Would I be available to walk with Emma?”
 “I made it,” Ronald proudly reports. “There was no way I wasn’t going to walk with her. This year hasn’t gone the way she had hoped. As frustrating as it is for her, it’s frustrating for us as parents. This is not the way we wanted her to close out of high school. When you have kids, you imagine certain events in certain ways. One thing that I have been clobbered over the head with this year is that things often don’t go the way we want. The crowd at the game were parents and siblings of seniors on the various teams, so it wasn’t the great celebration that we had hoped. At the end of the day, Erin was on one side, me on the other, and Emma between us. With Rachel watching from the stands, it didn’t matter who else was there. Our little family was there, and being together, when just a month ago everything was in question, was all that mattered.”
“I made it,” Ronald proudly reports. “There was no way I wasn’t going to walk with her. This year hasn’t gone the way she had hoped. As frustrating as it is for her, it’s frustrating for us as parents. This is not the way we wanted her to close out of high school. When you have kids, you imagine certain events in certain ways. One thing that I have been clobbered over the head with this year is that things often don’t go the way we want. The crowd at the game were parents and siblings of seniors on the various teams, so it wasn’t the great celebration that we had hoped. At the end of the day, Erin was on one side, me on the other, and Emma between us. With Rachel watching from the stands, it didn’t matter who else was there. Our little family was there, and being together, when just a month ago everything was in question, was all that mattered.”
The Support
To be approved for organ transplantation, patients must undergo a lot of testing. Some of that testing involves a social worker and psychology visits to ensure that the patient is mentally capable of going through a major surgery and organ transplantation. Another aspect is that the patient needs primary and secondary support after surgery.
“Even before surgery, it starts with making sure that the organ recipient has a good mindset and good support at home,” says Dr. Haithcock. “They will need help to get them through a big ordeal of an operation. Ronald was very energetic going into the operating room. Even though he did have a lull with the mental heaviness of the surgery, the support of his family and friends, as well as his enthusiasm, played a role in his rapid recovery.”
 Thru the entire experience, Ronald felt supported along his journey. “When I was a kid,” remembers Ronald, “I used to imagine myself winning a major award and thanking people. It seemed like a simple thing to do. You walk up, take the trophy, and you thank those who assisted you. Now, having grown (and realizing that awards are rich people patting themselves on their backs), I can’t do it. There is no way I can thank everyone for their outpouring of support and kind words. We are so thankful to everyone who dropped off a meal, snacks for the hospital visits, or just offered up positive vibes.”
Thru the entire experience, Ronald felt supported along his journey. “When I was a kid,” remembers Ronald, “I used to imagine myself winning a major award and thanking people. It seemed like a simple thing to do. You walk up, take the trophy, and you thank those who assisted you. Now, having grown (and realizing that awards are rich people patting themselves on their backs), I can’t do it. There is no way I can thank everyone for their outpouring of support and kind words. We are so thankful to everyone who dropped off a meal, snacks for the hospital visits, or just offered up positive vibes.”
“From the start, everyone I met with UNC Hospitals was wonderful.,” says Ronald. “Maybe it’s because I was basically a dead man walking, but everyone seemed interested in my welfare and concerned for me. This feeling of concern was evident from parking attendants to the surgical staff. I truly felt as if I had an entire team working for me and cheering me on. There is little doubt in my mind that my successful outcome has been because of the care I received at UNC. Of course, that wonderful care didn’t come without some frustrations. It was frustrating to be constantly woken in the middle of the night or to be constantly checked on while trying to heal, but it was a necessary thing. Intellectually, I knew it. Emotionally, I just wanted to sleep. After my transplant, the folks in the dining department worked to make sure that all of my meals were free from gluten so as not to aggravate my celiac disease. This little detail was critical in my healing. The nurses in the ICU and the step-down unit were top-notch. I have nothing but great things to say about them. I don’t remember the name of my night nurse in step-down, but she was especially wonderful. She was tireless in her efforts to not only provide me with the care I needed but to help me find the comfort I craved. It truly was a revolving door of providers but it was evident that it was a team effort. I was fortunate to be on the receiving end of that care.”
In His Own Words
Ronald has written a book about his journey through the lung transplant process. Check it out.