First Patient at UNC Hospitals to Receive a Double Lung Transplant Due to COVID-19 Diagnosis
Effect of COVID-19
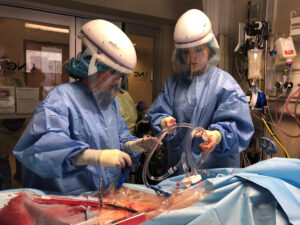
In May 2021, there were more than 3 million deaths worldwide from COVID-19. By December, that number increased to more than 5.2 million lives lost to the virus. COVID-19 is a respiratory disease that can cause various symptoms, including difficulty breathing, headache, fever, chills, cough, loss of taste or smell, muscle or body aches, and more. Those symptoms can range from mild to severe.
SARS-CoV-2, the virus that causes COVID-19, is part of the coronavirus family. The virus enters the body by coming into contact with the mucous membranes that line the nose, mouth, and eyes. The virus enters a healthy cell and uses the cell to make new virus parts. It multiplies, and the new viruses infect nearby cells. As the virus infects the respiratory tract, the immune system fights back, causing the lungs and airways to swell and become inflamed.
According to WebMD, “In critical COVID-19 — about 5% of total cases — the infection can damage the walls and linings of the air sacs in the lungs. As the body tries to fight it, the lungs become more inflamed and fill with fluid. This can make it harder for them to swap oxygen and carbon dioxide.”
The virus can eventually cause irreversible damage to the lungs that conventional therapy cannot fix.
Severe COVID-19 on the Lungs
 On April 24, 2021, Tolisha Alexander got married, an exciting and joyous time in her life. The newlyweds were excited to move into one home, blending their families. Tolisha was also thrilled to start a new job as a Dental Assistant II. Then in May, COVID-19 made its way through her entire family, most of whom experienced mild symptoms.
On April 24, 2021, Tolisha Alexander got married, an exciting and joyous time in her life. The newlyweds were excited to move into one home, blending their families. Tolisha was also thrilled to start a new job as a Dental Assistant II. Then in May, COVID-19 made its way through her entire family, most of whom experienced mild symptoms.
Tolisha remembers feeling unwell around May 24. “Well, I knew something was wrong. I just didn’t know exactly what because I’d never experienced anything like it before. It felt like a bad case of the flu. I’ve had the flu one time in my life, which was horrible, so I kind of knew I had something like that, but it was ten times worse.”
On May 29, Tolisha woke up with difficulty breathing, unable to even walk to the bathroom. Her husband called an ambulance to transport her to Vidant Hospital in Greenville, NC.
Tolisha spent two months in their facility, their team trying different treatments to help her lungs. While she had no other symptoms, the infection targeted her lungs and did irreparable damage. Her oxygen level dropped to 20%, and she required intubation so a machine could help her breathe. The team at Vidant contacted UNC in Chapel Hill to discuss other options.

“She had undergone conventional therapy which showed no improvement of her lung function,” explains Benjamin Haithcock, Surgical Director of the UNC Lung Transplant Program. “In addition, she required significant oxygen support, and we did not believe conventional therapy was going to be successful. She would need extraordinary measures.”
Tolisha was airlifted to UNC Medical Center in Chapel Hill in late July. After assessing her lungs, the team evaluated her and decided to consider her for a lung transplant. She would need a double lung transplant. “My lungs looked like I’ve been smoking for 20 years,” says Tolisha. “That’s how Dr. Haithcock explained it to me, but I’ve never smoked in my life.”
She was also placed on extracorporeal membrane oxygenation (ECMO), a machine similar to the heart-lung by-pass machine used in open-heart surgery. It pumps and oxygenates a patient’s blood outside the body, allowing the lungs to rest. When connected to ECMO, blood flows through tubing to an artificial lung in the machine that adds oxygen and takes out carbon dioxide; then the blood is warmed to body temperature and pumped back into your body.
Tolisha’s experience on ECMO was quite different from other patients. While most patients are sedated and unable to move on ECMO, the transplant team uses it differently. “We have done this for several patients,” says Dr. Haithcock. “In her case, we use ECMO as a bridge to transplant. We place the ECMO tubes through the neck. This allows the patient not to remain still. It also means patients don’t have to be sedated. Instead, they have the freedom to get up and move. We can completely support someone’s lungs while allowing them the mobility to move around and participate in activities. This helps us better evaluate these individuals. They can talk, interact, and eat, even as their lungs are damaged.”
Tolisha spent much of her free time doing laps around the hospital, visiting Starbucks on the ground floor of the cancer hospital, and keeping her body moving. “I was very functional on the ECMO machine,” recalls Tolisha. “I think being active before my surgery helped me in my recovery too.”
Due to the extensive damage to her lungs, Tolisha was high on the transplant list. However, to find the best match, she had to undergo multiple plasma exchanges, meaning her plasma was removed from her body, and donor plasma replaced it. This helped her immune system prepare for the transplant so her body would not reject the new lungs.
First COVID-19 Lung Transplant Patient
 On August 10, Tolisha was the first UNC patient to undergo a lung transplant due to COVID-19. She underwent a successful 11-hour double lung transplant surgery. She was discharged two weeks later to the SECU family house at UNC Hospitals, where she remained until the end of October, when she could finally go home. Her recovery included weekly physical therapy and occupational therapy appointments to help her grow strong enough to return home to Greenville.
On August 10, Tolisha was the first UNC patient to undergo a lung transplant due to COVID-19. She underwent a successful 11-hour double lung transplant surgery. She was discharged two weeks later to the SECU family house at UNC Hospitals, where she remained until the end of October, when she could finally go home. Her recovery included weekly physical therapy and occupational therapy appointments to help her grow strong enough to return home to Greenville.
In June 2020, Ankit Bharat, MD, chief of thoracic surgery and surgical director of lung transplantation and respiratory ECMO at Northwestern, performed a bilateral lung transplant on the first person in the US known to have undergone the procedure to treat COVID-19. In an article published June 21, 2021, by JAMA, “According to data from the United Network for Organ Sharing (UNOS), the nonprofit organization that manages the US organ transplant system, 134 lung transplants have been reported in the US for patients with COVID-19 through May 21. Among them, 82 patients had ARDS, 48 had developed pulmonary fibrosis, and 4 had unspecified lung failure due to COVID-19. In addition, one heart-lung transplant has been performed for COVID-19–related pulmonary fibrosis and heart failure. As of May 28, 22 patients with COVID-19–related lung failure were still on the lung transplant wait-list.”

Effects on People’s Lives
Research continues to be done on COVID-19 and its lasting effects on the lungs and the patients who are still recovering from it. “I think we will see more COVID patients, especially what has been described as the long haulers of COVID,” predicts Dr. Haithcock. “They are individuals with progressive lung disease, previously damaged lungs, smokers, and others with severe and catastrophic lung damage that can’t be reversed with the best medical treatments. UNC has all the resources to treat these patients. In Tolisha’s case, the team worked on all aspects of her health to get her well. Nurses helped her get on her feet. Security and other providers helped get her moving, sit outside, enjoy the sun, and play UNO while still receiving the critical care life-saving measure of ECMO and a lung transplant.”
“I think people downplay COVID,” says Tolisha. “I went from being a healthy adult who had a good career, just got married, getting used to a blended family, just moved into a new house, to an adult that can’t work. My husband and I just got married, so we spent five months in the hospital on our honeymoon. Not being able to work, that’s really affected me a lot. I’m glad to be alive. I thank God for that, but it is a life-changing experience all the way around.”
Due to COVID-19, Tolisha is out of work and focused on making a full recovery. If anyone would like to donate to help Tolisha and her family during this very challenging time, you can see her GoFundMe campaign. https://charity.gofundme.com/o/en/campaign/nft-tolishasolis
Recovery from COVID-19 poses a new set of challenges for patients and physicians alike. The UNC COVID Recovery Clinic serves as a central resource to provide medical care for COVID-19 survivors who have ongoing health effects.
An estimated 10 – 30% of COVID-19 survivors will experience lingering symptoms or health effects, a condition is frequently known as “Long COVID.” The most common persistent symptoms include fatigue, shortness of breath, weakness, headaches, “brain fog” (reduced attention or memory), anxiety, and depression.
“I do want to personally thank all the doctors and the nurses and everybody that really helped me,” says Tolisha. “The Cardiothoracic and Vascular Intensive Care Unit (CVTICU) was an awesome experience. I know it’s surprising because most people don’t think of it that way, but the nurses and doctors were amazing. I don’t feel like I would have made it if I hadn’t come to UNC. I also want to thank God first and my family and friends and especially my husband Warren for being by my side the whole way.”