Twenty four percent  of patients reporting a penicillin allergy had their allergy label removed after a five-minute pharmacy screening.
of patients reporting a penicillin allergy had their allergy label removed after a five-minute pharmacy screening.
On September 28, 1928, Alexander Fleming discovered penicillin. To commemorate this momentous discovery, every year on September 28th, we celebrate National Penicillin Allergy day to raise awareness that carrying a penicillin allergy label may negatively affect a patient’s health when it is not accurate.
Even though 10% of the U.S. population believes they have a penicillin allergy, less than 1% of the population is truly allergic. For the 9 out of 10 patients that are no longer (or never were) allergic, the allergy “label” on their medical record can lead to a host of negative consequences. They are often prescribed alternative antibiotics that are more expensive than penicillin, putting them at greater risk for developing multi-drug resistant infections. Additionally, patients with a penicillin allergy have more frequent and longer hospitalizations compared to non-allergic patients. Evaluating patients’ penicillin allergies for penicillin tolerance can alleviate burdens associated with a true allergy.
Allergists play a significant role in allergy evaluation at an estimated cost of $40 for some insured patients up to $700 for an uninsured patient paying out of pocket. But Dr. Renae Boerneke, clinical pharmacist practitioner, and Dr. Mildred Kwan, allergist, found a way to make allergy evaluation more accessible. They developed a process to conduct allergy assessments using an Epic dot phrase and risk stratification chart. Instead of requiring the expertise of an allergist in all cases, the evaluation can be carried out by a pharmacist or provider with the step-by-step tools. Based on screening questions, the patient may require an additional visit with an allergist. However, Boerneke found that pharmacists or non-allergist providers were able to de-label one in four patients screened, with no additional allergist visit needed. The change saved time and money for these patients, compared to evaluation using an allergist alone.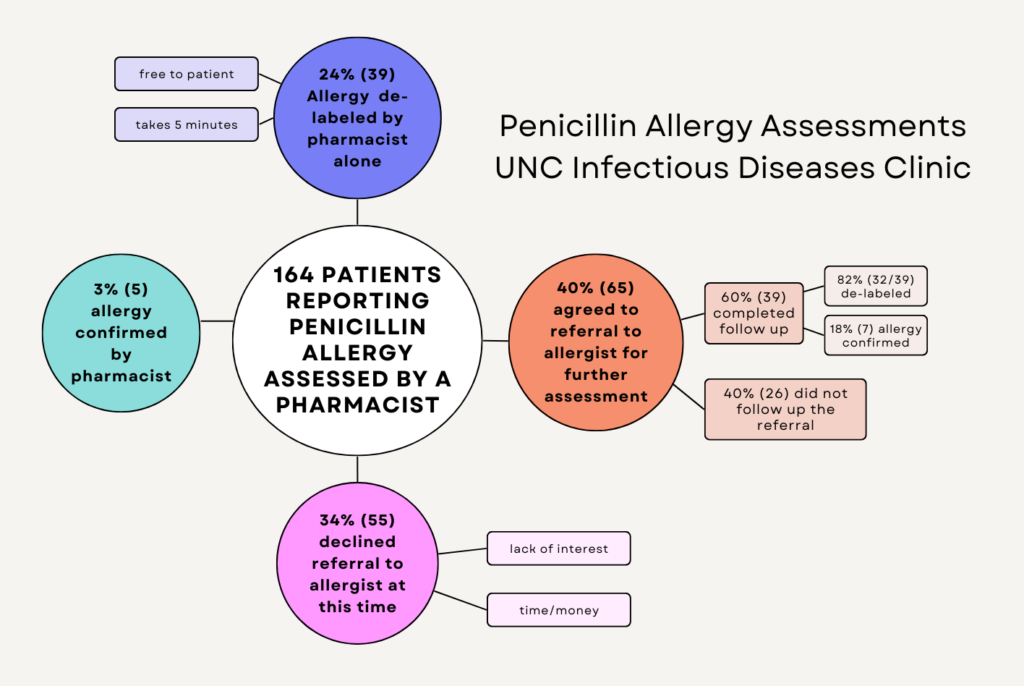
Over the last several years, 164 patients at the UNC Infectious Diseases Clinic participated in penicillin allergy assessments, resulting removal of penicillin allergy in 43% (71/164) of patients assessed. Nearly 24% (39) required only a brief pharmacist assessment for their allergy label to be removed. “A small number–five patients–had true allergies to penicillin confirmed during the assessment, so there was no change to their medical records,” Boerneke said.
The remaining patients required further evaluation by an allergist. A pharmacist made a referral for those interested in continuing at their own expense. Patients also had to be classified as low-risk (and therefore able to be evaluated using an oral amoxicillin graded challenge) or moderate-to-high-risk (assessed with a penicillin skin test followed by oral challenge) according to the screening questions. Of the patients who completed a second assessment with an allergist, 82% (32) were de-labeled, and the remaining 18% (7) had their allergy confirmed.
A meaningful proportion of de-labeled patients (43%) went on to receive a penicillin-class antibiotic, and only one patient (1%) experienced a mild delayed-onset rash to amoxicillin-clavulanic acid after previously passing the oral amoxicillin challenge. No other significant adverse events after penicillin use were documented.![]()
A penicillin allergy assessment tool kit is available to help train non-allergy providers to incorporate this important practice into their patient care. In under five minutes, a simple assessment can lead to improvements in patients’ health and healthcare expenditures, while potentially slowing the spread of antibiotic resistance.
Those interested in learning more may contact Renae.Boerneke@unchealth.unc.edu and Mildred.Kwan@med.unc.edu.