 *
*
Over five+ years at UNC, Ophthalmology Assistant Professor of Research Hua Mei, PhD, has brought wet lab capacity a step closer to fostering translational treatment of corneal and anterior segment diseases. Her laboratory’s translational framework is leading the way in developing the first FDA-approved, anti-fibrotic drug therapy to treat and prevent injury-induced corneal scarring, a leading cause of blindness that affects five+ million people worldwide. 
Dr. Mei noted: “Eye specialists can only mitigate damage to eyesight from corneal wounding through removing foreign bodies, providing eye patches, controlling root-cause diseases and treating infections with topical antibiotics and analgesics. An on-market, anti-fibrotic drug therapy would enable those affected to prevent or reduce corneal scar formation through boosting re-epithelialization and reducing myofibroblast transformation in a wounded cornea.”
Dr. Mei’s investigative path in corneal scarring drug discovery began by using single-cell RNA sequencing to identify two distinctive populations of limbal stem cells (corneal epithelial stem cells). Each limbal stem cell type secretes different signaling molecules. Combined in drug therapy, however, both may facilitate corneal epithelial regeneration and re-establish barrier functions that are the first line of cellular defense against chemical, biological, and physical threats in fighting corneal pathological conditions.
Mei lab discovery of using protein coding gene NBL1 (a BMP antagonist) to inhibit corneal fibrosis and scar formation after wounding in mice and cultured human corneas has led to study of its potential for drug therapy development. Both secured patents and others in writing are advancing her lab’s exclusive investigative rights in applying corneal epithelial stem cell discoveries to novel application of self-administered eye drops to treat corneal limbal stem cell deficiency, corneal scar, corneal neovascularization, and dry eye disease.
Dr. Mei concluded: “My team’s pre-clinical strides will one day provide the general public and those in higher-risk occupations access to a drug therapy to treat an all-too-common type of ocular trauma. Military personnel and construction workers have higher rates of corneal damage. Domestically, corneal scrapes and store-shelf products with damaging chemicals spilled into eyes affect many adults and children. Without anti-fibriotic therapies on the market to aid healing of corneal injuries, scar tissue that can worsen an individual’s eyesight will almost inevitably form.”
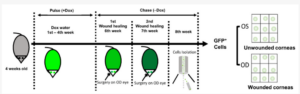
* In the June 2022 issue of Cells, Dr. Hua Mei’s laboratory conducted corneal wound-healing experimentation in mouse models using single-cell RNA sequencing as a translational step toward studying wound healing in cultured human corneas. Hua lab discovery of several limbal stem cell and limbal progenitor cell types under normal homeostasis has established a translational framework for further study of the dynamics of corneal epithelial regeneration and wound healing.