Specialty Areas:
Lung stem/progenitor cells, airway mucins and inflammation in health and diseases.
About:
Dr. Gang Chen is an assistant professor in the Marsico Lung Institute and Cystic Fibrosis Research Center. He is also affiliated with the faculty of the Division of Pediatric Pulmonology at the Department of Pediatrics, Cell Biology and Physiology (CBP) Curriculum and the Biological & Biomedical Sciences Program (BBSP), UNC at Chapel Hill. Dr. Chen received his B.S. and M.S degrees both from Yangzhou University, China, his Ph.D. from the Molecular and Developmental Biology Graduate Program of Cincinnati Children’s Hospital, and his postdoctoral training from both the Cincinnati Children’s Hospital and Cystic Fibrosis Center of UNC at Chapel Hill.
Academic Experience & Training:
2021-present Assistant Professor (Tenure Track)
Marsico Lung Institute/Cystic Fibrosis Research Center, University of North Carolina at Chapel Hill
2014-2020 Research Associate
Marsico Lung Institute/Cystic Fibrosis Research Center, University of North Carolina at Chapel Hill
2013-2014 Postdoctoral Fellow
Cystic Fibrosis Research Center, University of North Carolina at Chapel Hill
2011-2012 Postdoctoral Fellow
Perinatal Institute, Cincinnati Children’s Hospital
2004-2010 Graduate Student (PhD)
Molecular and Developmental Biology Graduate Program
Cincinnati Children’s Hospital and University of Cincinnati
2002-2003 Research Assistant
Institute of Laboratory Animal Sciences, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing, China
1999-2002 Graduate Student (MS)
College of Veterinary Medicine, Yangzhou University, Yangzhou, China
1995-1999 Undergraduate Student (BS)
College of Bioscience and Biotechnology, Yangzhou University, Yangzhou, China
Honors & Awards:
2012-2013 American Lung Association Senior Research Training Fellowship
Research Experience:
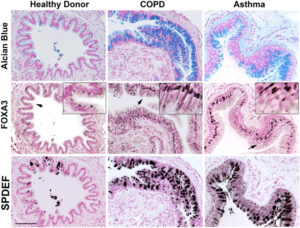
Dr. Chen was trained as a molecular and developmental biologist during his PhD and an early postdoc training with Jeff Whitsett, MD, at Cincinnati Children’s Hospital Medical Center. Specifically, he studied the role of respiratory epithelial transcription factors in controlling lung branching morphogenesis, development, and roles of epithelial progenitor/stem cells during injury and repair. His thesis work resulted in the identification and explication of a number of important genes and a key transcription network including SPDEF, FOXA3 (Fig. 1,2), FOXA2 and NKX2.1, delineating their abilities to work as gateways that modulate MUC5AC expression and mucus production in airway goblet cells in response to Th2-dominant pulmonary inflammation that relates to allergic asthma and antiviral responses in the lung.
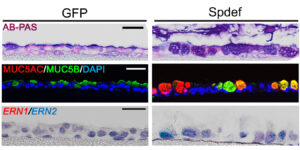
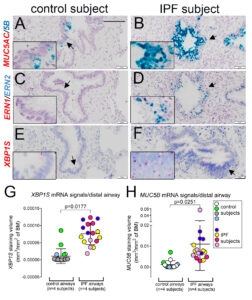
Since joining the lab of Richard Boucher, MD, in the Marsico Lung Institute at UNC at Chapel Hill, Dr. Chen has been working to discover the transcriptional regulation of MUC5B, a major respiratory tract secretory mucin required at baseline for health, but often excessively produced in chronic muco-obstructive pulmonary diseases, like cystic fibrosis (CF), idiopathic pulmonary fibrosis (IPF), chronic bronchitis and chronic obstructive pulmonary disease (COPD). He and colleagues identified a novel pathway leading to excessive MUC5B production in the IPF lung that is mediated by the SPDEF-ERN2-XBP1S axis, linking the unfolded protein response (UPR) with mucin production in the distal airway epithelia of IPF (Fig. 3). Profoundly, this work for the first time explained the differential regulation of the MUC5B promoter polymorphism rs35705950, the strongest genetic association with pathogenesis of IPF, by the ER stress transcription factor XBP1S, a potential therapeutic target.
Dr. Chen has also committed to study abnormal mucus hyperconcentration and obstruction in CF. He and colleagues have dissected the precise transcriptional mechanisms that regulate excessive mucin production in CF airways, dominated by non-TH2 inflammation that results in hyperproduction of regional-specific mucin expression patterns, i.e., MUC5AC/MUC5B-mixed in proximal vs. MUC5B-dominated in distal CF airways. They identified that proinflammatory and profibrotic cytokine interleukin 1β (IL1β) is the dominant factor presented in CF airway secretions that causes the abnormal mucus hyperconcentration phenotype in the CF lung. They developed genetic tools to block the function of IL1β receptor (IL1R1) to suppress excessive mucin production, as well as inflammatory responses by CRISPR-Cas9 technology or by the pharmacological inhibitor anakinra in primary human bronchial epithelial cells isolated from normal and CF lungs.
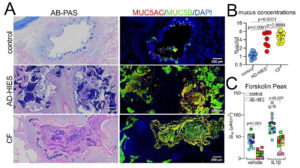
In close collaboration with Drs. Richard Boucher and Kenneth Olivier at UNC, Drs. Alexandra Freeman and Kevin Fennelly at NIH, and Dr. Peter Mogayzel at John Hopkins, Dr. Chen has also led a study of the rare genetic disease autosomal dominant hyper-IgE syndrome (AD-HIES). AD-HIES is primarily an immunological disease, caused by mutations in the STAT3 protein which lead to IL22/TH17 cell differentiation deficiency, and it is often associated with recurrent pulmonary infection, the leading cause of mortality in this disease. Using primary patients’ airway cells, biopsy specimens, and STAT3 CRISPR/Cas9 gene-edited normal primary cells, this team has identified the molecular and cellular mechanisms underlying the STAT3 mutations caused mucociliary clearance defects and mucus obstruction (Fig. 4). These epithelial abnormalities lead to defective innate host defense and failure in clearance of infection, which in turn lead to chronic inflammation, lung structural damage and loss of lung function.
Selected Bibliography:
- Schworer SA, Murano H, Dang H, Markovetz MR, Saito M, Kato T, Asakura T, Chen G, Gilmore RC, Morton LC, van Heusden C, Chua M, Strickler E, Wisniewski ZY, Crisp G, Mitchell E, Doherty KA, Mastan S, Trejo Bittar HE, Cody BA, Trudeau JB, De la Cruz G, Ralph LM, Askin FB, Panettieri RA Jr, Koziol-White CJ, Byrd KM, Livraghi-Butrico A, O’Neal WK, Randell SH, Wenzel SE, Okuda K, Boucher RC Jr. Airway Epithelial Heterogeneity and Mucus Plugging in Asthmatic Bronchioles. Am J Respir Crit Care Med. 2026 Feb;212(2):209-226. doi: 10.1164/rccm.202409-1849OC. PMID: 40986379. PMCID: PMC12668797.
- Sun L, Walls SA, Dang H, Quinney NL, Sears PR, Sadritabrizi T, Hasegawa K, Okuda K, Asakura T, Chang X, Zheng M, Mikami Y, Dizmond FU, Danilova D, Zhou L, Deshmukh A, Cholon DM, Radicioni G, Rogers TD, Kissner WJ, Markovetz MR, Guhr Lee TN, Gutay MI, Esther CR Jr, Chua M, Grubb BR, Ehre C, Kesimer M, Hill DB, Ostrowski LE, Button B, Gentzsch M, Robinson C, Olivier KN, Freeman AF, Randell SH, Vladar E, O’Neal WK, Boucher RC Jr, Chen G. STAT3-dependent Regulation of CFTR and Ciliogenesis Is Essential for Mucociliary Clearance and Innate Airway Defense in Hyper-IgE Syndrome. Am J Respir Crit Care Med. 2025 Oct;211(10):1951-1969. doi: 10.1164/rccm.202407-1415OC. PMID: 40315437. PMCID: PMC12555045.
- Pickles RJ, Chen G, Randell SH. Enhanced susceptibility of pediatric airway epithelium to respiratory syncytial virus infection. J Clin Invest. 2024 Nov 1;134(21):e185689. doi: 10.1172/JCI185689. PMID: 39484717; PMCID: PMC11527439.
- Asakura T, Okuda K, Chen G, Dang H, Kato T, Mikami Y, Schworer SA, Gilmore RC, Radicioni G, Hawkins P, Barbosa Cardenas SM, Saito M, Cawley AM, De la Cruz G, Chua M, Alexis NE, Masugi Y, Noone PG, Ribeiro CMP, Kesimer M, Olivier KN, Hasegawa N, Randell SH, O’Neal WK, Boucher RC. Proximal and Distal Bronchioles Contribute to the Pathogenesis of Non-Cystic Fibrosis Bronchiectasis (NCFB). Am J Respir Crit Care Med. 2024 Feb 15;209(4):374-389. doi: 10.1164/rccm.202306-1093OC. PMID: 38016030. PMCID: PMC10878387.
- Donoghue LJ, Markovetz MR, Morrison CB, Chen G, McFadden KM, Sadritabrizi T, Gutay MI, Kato T, Rogers TD, Snead JY, Livraghi-Butrico A, Button B, Ehre C, Grubb BR, Hill DB, Kelada SNP. BPIFB1 loss alters airway mucus properties and diminishes mucociliary clearance. Am J Physiol Lung Cell Mol Physiol. 2023 Dec 1;325(6):L765-L775. doi: 10.1152/ajplung.00390.2022. PMID: 37847709. PMCID: PMC11068428.
- Mikami Y, Grubb BR, Rogers TD, Dang H, Asakura T, Kota P, Gilmore RC, Okuda K, Morton LC, Sun L, Chen G, Wykoff JA, Ehre C, Vilar J, van Heusden C, Livraghi-Butrico A, Gentzsch M, Button B, Stutts MJ, Randell SH, O’Neal WK, Boucher RC. Chronic airway epithelial hypoxia exacerbates injury in muco-obstructive lung disease through mucus hyperconcentration. Sci Transl Med. 2023 Jun 7;15(699):eabo7728. doi: 10.1126/scitranslmed.abo7728. PMID: 37285404. PMCID: PMC10664029.
- Schworer SA, Chason KD, Chen G, Chen J, Zhou H, Burbank AJ, Kesic MJ, Hernandez ML. Interleukin-1 receptor antagonist attenuates pro-inflammatory responses to rhinovirus in airway epithelium. J Allergy Clin Immunol. 2023 Jun;151(6):1577-1584.e4. doi: 10.1016/j.jaci.2023.01.015. PMID: 36708816. PMCID: PMC10257744.
- Kato T, Asakura T, Edwards CE, Dang H, Mikami Y, Okuda K, Chen G, Sun L, Gilmore RC, Hawkins P, De la Cruz G, Cooley MR, Bailey AB, Hewitt SM, Chertow DS, Borczuk AC, Salvatore S, Martinez FJ, Thorne LB, Askin FB, Ehre C, Randell SH, O’Neal WK, Baric RS, Boucher RC; NIH COVID-19 Autopsy Consortium. Prevalence and Mechanisms of Mucus Accumulation in COVID-19 Lung Disease. Am J Respir Crit Care Med. 2022 Dec 1;206(11):1336-1352. doi: 10.1164/rccm.202111-2606OC. PMID: 35816430. PMCID: PMC9746856.
- Hsu AP, Korzeniowska A, Aguilar CC, Gu J, Karlins E, Oler AJ, Chen G, Reynoso GV, Davis J, Chaput A, Peng T, Sun L, Lack JB, Bays DJ, Stewart ER, Waldman SE, Powell DA, Donovan FM, Desai JV, Pouladi N, Long Priel DA, Yamanaka D, Rosenzweig SD, Niemela JE, Stoddard J, Freeman AF, Zerbe CS, Kuhns DB, Lussier YA, Olivier KN, Boucher RC, Hickman HD, Frelinger J, Fierer J, Shubitz LF, Leto TL, Thompson III GR, Galgiani JN, Lionakis MS, Holland SM. Immunogenetics associated with severe coccidioidomycosis. JCI Insight. 2022 Nov 22;7(22):e159491. doi: 10.1172/jci.insight.159491. PMID: 36166305. PMCID: PMC9746810.
- Okuda K, Dang H, Kobayashi Y, Carraro G, Nakano S, Chen G, Kato T, Asakura T, Gilmore RC, Morton LC, Lee RE, Mascenik T, Yin WN, Barbosa Cardenas SM, O’Neal YK, Minnick CE, Chua M, Quinney NL, Gentzsch M, Anderson CW, Ghio A, Matsui H, Nagase T, Ostrowski LE, Grubb BR, Olsen JC, Randell SH, Stripp BR, Tata PR, O’Neal WK, Boucher RC. Secretory Cells Dominate Airway CFTR Expression and Function in Human Airway Superficial Epithelia. Am J Respir Crit Care Med. 2021 May 15;203(10):1275-1289. PMID: 33321047. PMCID: PMC8456462.
- Hou YJ, Okuda K, Edwards CE, Martinez DR, Asakura T, Dinnon III KH, Kato T, Lee RE, Yount BL, Mascenik TM, Chen G, Olivier KN, Ghio A, Tse LV, Leist SR, Gralinski LE, Schäfer A, Dang H, Gilmore R, Fulcher L, Livraghi-Butrico A, Nicely NI, Cameron M, Cameron C, Kelvin DJ, de Silva A, Margolis DM, Markmann A, Bartelt L, Zumwalt R, Martinez FJ, Salvatore SP, Borczuk A, Tata PR, Sontake V, Kimple A, Jaspers I, O’Neal WK, Randell SH, Boucher RC, Baric RS. SARS-CoV-2 Reverse Genetics Reveals a Variable Infection Gradient in the Respiratory Tract. Cell. 2020 Jul 23;182(2):429-446.e14. PMID: 32526206; PMCID: PMC7250779.
- Chen G, Sun L, Kato T, Okuda K, Martino MB, Abzhanova A, Lin JM, Gilmore RC, Batson B, Volmer AS, O’Neal YK, Dang H, Deng Y, Randell SH, Button B, Livraghi-Butrico A, Kesimer M, Ribeiro CMP, O’Neal WK, Boucher RC. IL-1β dominates the promucin secretory cytokine profile in cystic fibrosis. J Clin Invest. 2019 Oct 1;129(10):4433-4450. PMID: 31524632; PMCID: PMC6763234.
- Chen G, Ribeiro CMP, Sun L, Okuda K, Kato T, Gilmore RC, Martino MB, Dang H, Abzhanova A, Lin JM, Hull-Ryde EA, Volmer AS, Randell SH, Livraghi-Butrico A, Deng Y, Scherer PE, Stripp BR, O’Neal WK, Boucher RC. XBP1S Regulates MUC5B in a Promoter Variant-Dependent Pathway in IPF Airway Epithelia. Am J Respir Crit Care Med 2019 Jul 15;200(2):220-234. PMID: 30973754; PMCID: PMC6635783.
- Okuda K, Chen G, Subramani DB, Wolf M, Gilmore RC, Kato T, Radicioni G, Kesimer M, Chua M, Dang H, Livraghi-Butrico A, Ehre C, Doerschuk CM, Randell SH, Matsui H, Nagase T, O’Neal WK, Boucher RC. Localization of Secretory Mucins MUC5AC and MUC5B in Normal/Healthy Human Airways. Am J Respir Crit Care Med 2019 Mar 15;199(6):715-727. PMID: 30352166; PMCID: PMC6423099.
- Chen G, Volmer AS, Wilkinson KJ, Deng Y, Jones LC, Yu D, Bustamante-Marin XM, Burns KA, Grubb BR, O’Neal WK, Livraghi-Butrico A, Boucher RC. Role of Spdef in the Regulation of Muc5b Expression in the Airways of Naïve and Muco-obstructed Mice. Am J Respir Cell Mol Biol 2018; 59(3): 383-396. PMID: 29579396; PMCID: PMC6189647.
- Yu D, Saini Y, Chen G, Ghio AJ, Dang H, Burns KA, Wang Y, Davis RM, Randell SH, Esther CR, Jr., Paulsen F, Boucher RC. Loss of beta Epithelial Sodium Channel Function in Meibomian Glands Produces Pseudohypoaldosteronism 1-Like Ocular Disease in Mice. Am J Pathol 2018; 188: 95-110. PMID: 29107074; PMCID: PMC5745530.
- Donoghue LJ, Livraghi-Butrico A, McFadden KM, Thomas JM, Chen G, Grubb BR, O’Neal WK, Boucher RC, Kelada SNP. Identification of trans Protein QTL for Secreted Airway Mucins in Mice and a Causal Role for Bpifb1. Genetics 2017; 207: 801-812. PMID: 28851744; PMCID: PMC5629340.
- Esther CR, Jr., Hill DB, Button B, Shi S, Jania C, Duncan EA, Doerschuk CM, Chen G, Ranganathan S, Stick SM, Boucher RC. Sialic acid-to-urea ratio as a measure of airway surface hydration. American journal of physiology Lung cellular and molecular physiology 2017; 312: L398-L404. PMID: 28062483; PMCID: PMC5374301.
- Rajavelu P, Chen G, Xu Y, Kitzmiller JA, Korfhagen TR, Whitsett JA. Airway epithelial SPDEF integrates goblet cell differentiation and pulmonary Th2 inflammation. J Clin Invest 2015; 125: 2021-2031. PMID: 25866971; PMCID: PMC4463206.
- Chen G, Korfhagen TR, Karp CL, Impey S, Xu Y, Randell SH, Kitzmiller J, Maeda Y, Haitchi HM, Sridharan A, Senft AP, Whitsett JA. Foxa3 induces goblet cell metaplasia and inhibits innate antiviral immunity. Am J Respir Crit Care Med 2014; 189: 301-313. PMID: 24392884; PMCID: PMC3977731.
- Ren X, Shah TA, Ustiyan V, Zhang Y, Shinn J, Chen G, Whitsett JA, Kalin TV, Kalinichenko VV. FOXM1 promotes allergen-induced goblet cell metaplasia and pulmonary inflammation. Mol Cell Biol 2013; 33: 371-386. PMID: 23149934; PMCID: PMC3554115.
- Noah TK, Lo YH, Price A, Chen G, King E, Washington MK, Aronow BJ, Shroyer NF. SPDEF functions as a colorectal tumor suppressor by inhibiting beta-catenin activity. Gastroenterology 2013; 144: 1012-1023 e1016. PMID: 23376423; PMCID: PMC3738069.
- Marko CK, Menon BB, Chen G, Whitsett JA, Clevers H, Gipson IK. Spdef null mice lack conjunctival goblet cells and provide a model of dry eye. Am J Pathol 2013; 183: 35-48. PMID: 23665202; PMCID: PMC3702735.
- Wang IC, Snyder J, Zhang Y, Lander J, Nakafuku Y, Lin J, Chen G, Kalin TV, Whitsett JA, Kalinichenko VV. Foxm1 mediates cross talk between Kras/mitogen-activated protein kinase and canonical Wnt pathways during development of respiratory epithelium. Mol Cell Biol 2012; 32: 3838-3850. PMID: 22826436; PMCID: PMC3457538.
- Korfhagen TR, Kitzmiller J, Chen G, Sridharan A, Haitchi HM, Hegde RS, Divanovic S, Karp CL, Whitsett JA. SAM-pointed domain ETS factor mediates epithelial cell-intrinsic innate immune signaling during airway mucous metaplasia. Proc Natl Acad Sci U S A 2012; 109: 16630-16635. PMID: 23012424; PMCID: PMC3478616.
- Maeda Y, Chen G, Xu Y, Haitchi HM, Du L, Keiser AR, Howarth PH, Davies DE, Holgate ST, Whitsett JA. Airway epithelial transcription factor NK2 homeobox 1 inhibits mucous cell metaplasia and Th2 inflammation. Am J Respir Crit Care Med 2011; 184: 421-429. PMID: 21562130; PMCID: PMC3175541.
- Chen G, Wan H, Luo F, Zhang L, Xu Y, Lewkowich I, Wills-Karp M, Whitsett JA. Foxa2 programs Th2 cell-mediated innate immunity in the developing lung. J Immunol 2010; 184: 6133-6141. PMID: 20483781.
- Chen G, Korfhagen TR, Xu Y, Kitzmiller J, Wert SE, Maeda Y, Gregorieff A, Clevers H, Whitsett JA. SPDEF is required for mouse pulmonary goblet cell differentiation and regulates a network of genes associated with mucus production. J Clin Invest 2009; 119: 2914-2924. PMID: 19759516; PMCID: PMC2752084.
- Maeda Y, Suzuki T, Pan X, Chen G, Pan S, Bartman T, Whitsett JA. CUL2 is required for the activity of hypoxia-inducible factor and vasculogenesis. J Biol Chem 2008; 283: 16084-16092. PMID: 18372249; PMCID: PMC2414293.
- Park K-S, Korfhagen TR, Bruno MD, Kitzmiller JA, Wan H, Wert SE, Khurana Hershey GK, Chen G, Whitsett JA. SPDEF regulates goblet cell hyperplasia in the airway epithelium. J Clin Invest 2007; 117: 978-988. PMID: 17347682; PMCID: PMC1810569.
A full list of Gang Chen’s publication can be found at the following link:
https://www.ncbi.nlm.nih.gov/myncbi/1NO-gAEzLz0kH/bibliography/public/
