We hope that you might find some comfort during this unprecedented time knowing that we are continuing to work for you. COVID-19 is upending lives and day-to-day for all of us. Our faculty and staff are on the frontlines of the response, working hard to serve our patients in a time when proper physical and mental care are more important than ever. We are sharing with you some of our stories in leadership, courage, and compassion to provide you an inside look to how we are all in this together.
Working for You During COVID-19
UNC Family Medicine: Leadership, Courage, and Compassion during the time of COVID-19

We are doing all we can to get our community and state back on track, but we need your help. Your support along with others can make a difference, especially for those who are most vulnerable. Please consider supporting our work today.
Our Stories
Q&A with Erik Butler, DO, Assistant Professor
The following is a Q&A session with Erik Butler, DO, Assistant Professor. Dr. Butler came to UNC Family Medicine from private practice, and his interests lie in individual and community care; cardiovascular health, dermatology, musculoskeletal medicine, and disease prevention.

Q: Can you please give a brief description of your role during COVID-19? What is your day like?
A: My day to day work as a family medicine doctor and educator has definitely changed since the COVID pandemic started. I am taking care of patients in a variety of new ways that includes a mix of in-person visits, video and telephone visits as well as using MyUNCChart to stay in touch.
Q: What challenges are you facing?
A: Teaching medical students and residents during a pandemic has created a unique set of challenges. We have adjusted medical student experiences in Family Medicine to include telehealth visits, as well as in-person continuity clinic and urgent care. In March, my fundamental clinical skills class made up of first year medical students was switched to on-line remote learning. However, this semester we are back together again to practice their physical exam skills and clinical reasoning, and the student seem thrilled to restart their hands-on learning.
Q: In your opinion, what role has Family Medicine played throughout the pandemic crisis?
A: I feel like UNC Family Medicine has done a great job developing protocols to keep patients and staff safe while continuing to provide in-person care. It’s great that we can still see our patients when we need to.
Q: Do you have other personal reflections or comments?
A: Taking care of patients and giving medical students a meaningful experience has certainly been challenging for all during the COVID pandemic. I’ve been impressed by how everyone involved has made adjustments and done the best they can during such a difficult time. What’s clear is how we all need each other now more than ever and I’m grateful to be part of such a great team at Family Medicine.
Q&A with Chineme Enyioha, MD, MPH, Assistant Professor
The following is a Q&A session with Chineme Enyioha, MD, MPH, Assistant Professor. Dr. Enyioha’s research focuses on health disparities, decision science and examining factors that affect patients’ engagement in healthcare especially with chronic disease management.

Q: Can you please give a brief description of your role during COVID-19?
A: I am a clinician-researcher, which means that I see patients and take care of other clinical responsibilities while working on research projects related to chronic disease management and health disparities with a goal of bridging the disparities gap we have in healthcare.
Q: What is your day-to-day like?
A: It varies from day to day because of my other non-clinical activities such as my research. Some days are filled with research activities and virtual meetings. Other days are filled with clinical responsibilities, which include in person clinic sessions and virtual care. Some days are filled with a mixture or variety of clinic sessions, research, and other academic activities.
Q: What challenges are you facing?
A: One major challenge is the concern about patients who don’t have access to care for several reasons including the present pandemic. There is a limit to the type of care that can be provided virtually. In addition, many people feel the effect of the current situation in different ways that directly or indirectly affect their health. The healthcare system is constantly changing in order to provide the best care possible. This gives me hope.
Q: In your opinion, what role has Family Medicine played throughout the pandemic crisis?
A: Family Medicine has played a significant role during this pandemic. Our department has stepped up to the task in many ways – from redesigning the way in which we provide care to accommodate more patients in clinic and on the inpatient service, to providing virtual care/telemedicine while keeping staff and providers as safe as possible. Family Medicine at UNC has also been on the forefront by providing staffing for the respiratory diagnostic center and occupational health. Patients have also shown appreciation and gratitude that the Family Medicine Clinic is open to see them and address their health concerns in a timely manner.
Q: Do you have other personal reflections or comments?
A: Life, as we know it, has changed significantly. The current situation is a reminder that we should value the time we have with family, friends and colleagues. I always say, “take things one day at a time” and enjoy the moment you have now as much as you can while you hope for the best.
Alexa Mieses Malchuk, MD, MPH, on Health Equity and COVID-19

Dr. Mieses Malchuk is our Diversity Liaison and is the Co-Director of Curricular Innovation for Health Equity
As a child, I experienced health disparities first-hand. I was drawn to family medicine for the opportunity to achieve health equity for my patients. I have worked at the intersection of public health and clinical medicine for several years. Now more than ever before, COVID-19 has put a spotlight on health disparities that have existed for decades. As a result, there has been increased interest and momentum around issues related to social determinants of health more broadly.
For example, people of color are often at higher risk for disease and complications of disease as a result of systemic racism. This is no different for COVID-19. People of any color are also at risk for disease and disease complications based on socioeconomic status, immigration status, English proficiency and education (just to name a few social determinants of health). COVID-19 is no different. Poorer patients and patients of color are faring much worse than their wealthier, white counterparts when it comes to the likelihood of getting COVID-19 and ultimately dying from it.
When the pandemic first started, there were a lot of unknowns about the virus itself and the widespread PPE shortages throughout the nation. Therefore, telemedicine encounters skyrocketed. We began to provide care via video and telephone visits. We are still learning more and more about COVID-19 every day. However, now we have started to safely integrate in-person visits and procedures again via PPE for patients and the care team, and other policies that help ensure safety.
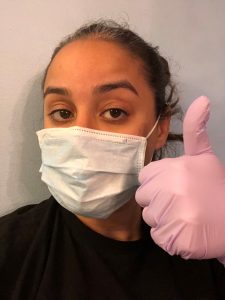
As a primary care physician, there have been several challenges. First, I am very concerned about my patients who were already marginalized and had limited access to care. I worry for their health. I also worry about folks who avoid seeking medical attention altogether for fear of contracting COVID-19 while in clinic or at the hospital. This can lead to treatable conditions getting even more out of control and becoming dangerous.
Primary care physicians are on the front lines of the pandemic in so many ways. Family physicians are trained to be the first point of contact in the healthcare system in emergency departments, clinics and hospitals. We treat acute illness like actual COVID-19 infections, but also provide comprehensive preventative healthcare services to keep people healthy throughout their lifetime.
The COVID-19 pandemic has transformed our professional and personal lives. It has changed the way we care for patients. It has emphasized the importance of public health. COVID-19 has altered the way we interact with loved ones. Perhaps a pleasant surprise is that this pandemic has created a greater sense of connectedness for us all.
Karen Halpert, MD, shares a Medical Director’s perspective
Karen Halpert, MD, is an assistant professor of Family Medicine and graduate of the UNC Family Medicine residency program. She serves as Medical Director at our Durham clinic, and throughout the course of the COVID-19 pandemic has been acting Medical Director of the Family Medicine Center in Chapel Hill as well.
What is the day-to-day like for you as Medical Director during this time, and for the FMC leadership team?
The FMC has a tremendous leadership team! During COVID-19, we have worked together to develop ever changing protocols to keep our patients, staff and providers safe. As a clinic, we have gone from seeing 100% of our patients in-person, to at our peak seeing almost 75% virtually! We are constantly adapting to patient needs. We now offer a balance of in-person, video or phone visits depending on what would work best for our patients. We heard that parents may be concerned about bringing their kids into

clinic for well-child checks, so we developed well-child clinic half-days. As a medical director, this has been an ever-evolving process that has involved all of our staff and providers stepping up! It has been an honor to serve with our staff, providers, and leadership team. Everyone is constantly thinking about how to improve our processes and keep people safe. I am also so grateful for our patients who have reached out and shared their support for our hard work!
What are some of the ways you have noticed our department stepping up or adapting amidst COVID-19?
Our department has stepped up in a lot of ways, but in clinic everyone has adapted to new processes that at one point seemed were changing twice a week! We have had attendings, residents, medical students and medical assistants stepping up to help screen patients in the parking lot. Everyone is adapting to virtual care and raising great points on how we can improve the processes. Our department was one of the early success stories for virtual care in the health care system! Our flexibility to care for our patients and work as a team clearly made this possible!
What future implications do you think this pandemic will have for Family Medicine, or health care overall?
The pandemic has certainly changed our processes and approach to virtual care (video and phone visits). It has been a great joy to be welcomed into patients’ homes, cars and offices via video visits. While we may still have some kinks, it has been a joy to still be able to take care of patients despite initial concerns of patients coming into clinic. While our clinic is opening up for more in-person visits, it is great to know that video or phone visits are still an easily accessible option that may help patients get care as their lives get busier! We know patients generally have to take time off from work, get a babysitter or set up a ride to come in for an appointment, so it is lovely to have the option to take care of you when and where it is convenient for the patient!
What is something you want our patients to know about our team and/or services during this time?
The FMC in Chapel Hill and Durham miss you! We love taking care of you and want you to know we are here for you. If you need to schedule an appointment, our schedules are opening up with more access to your primary care provider virtually or in-person. If you are still hesitant to come into our clinic, we would love to take care of you via video or phone visits! Our staff and leadership team are committed to your safety and are constantly looking at ways to improve our process and increase access to our services. If you have suggestions on how we can improve the care we provide, we would love to hear from you!
Dr. Timothy Daaleman reflects on disparities in the time of COVID-19
Timothy Daaleman, DO, MPH, is a Professor of Family Medicine at UNC-CH. His areas of focus include care of medically vulnerable populations and chronic illness care, social and cultural influences on chronic illness and end-of-life care, and aging and the life course. He is currently involved with the Orange County Partnership to End Homelessness, and offers his insight on the challenges and response COVID-19 has brought about.

Describe your role with the Orange County Partnership to End Homelessness in response to COVID-19?
I have been privileged to be part of the Orange County Homeless System COVID Coordination and Unsheltered Workgroups. The groups bring together government agencies, community-based homeless service providers, and other stakeholders to coordinate a system-level response to COVID-19 for people experiencing homelessness. I continue to be heartened by the commitment of the workgroup members in their responsiveness to our most vulnerable patients and am impressed with the teamwork and organizational acumen of the group.
What is your day-to-day like?
My day is filled with virtual meetings, clinical responsibilities, and academic work. Overall it has been a positive growth experience in which I have been rapidly upskilled in remote learning and virtual outpatient care, as well as in the redirection of my inpatient work to Hillsborough Hospital. Throughout such rapid change, I have maintained a daily practice of connecting with our committed patient care staff in the Family Medicine Center which keeps me grounded.
What challenges are you facing?
We live in a time-suspended world. The uncertainty generated by COVID-19 has upended planning for program development, grant proposals, and academic coursework.
In your opinion, what role has Family Medicine played throughout the pandemic crisis?
The pandemic has revealed the critical role of family medicine in the health care delivery system by highlighting the need for a broad clinical skill set, systems-level thinking, and teamwork across different clinical environments.
Do you have other personal reflections or comments?
During the pandemic I am often hearing, “every day is the same day” and “when will it end?” As physicians, we are trained in the art and science of prognosis – the likely course of an illness or injury – which has led me to reflect on how we view the concept of time. The ancient Greeks had different understandings of time; chronos or measured time and kairos or the right time that invites opportunity and change. The pandemic and death of George Floyd have brutally exposed the unjust disparities and systemic racism that are embedded in our individual and collective consciousness, and in our organizations. I believe that we are entering into a kairos moment.

Q&A with Margaret Helton, MD, Interim Chair of UNC Family Medicine and Medical Director of Carol Woods Retirement Community
The following is a Q&A session with Margaret Helton, MD, Interim Chair of UNC Family Medicine and Medical Director of Carol Woods Retirement Community. Her past leadership positions in the department include Vice Chair of Clinical Excellence, Associate Chair for Faculty Affairs, Director of Career Development Fellowship, Director of Operations, and Director of Maternal and Child Health, and she practices in full spectrum family medicine, women’s health, geriatrics, and end-of-life care.
Q: Can you please give a brief description of how your role has changed due to COVID-19?
A: My role as Chair has been to steady the ship as we sail through roiling waters. The early days in March and April felt like a firehose pointed at me all the time, with a barrage of new challenges every day. The key to maneuvering through these waters included tapping into our deep well of talent, listening, and taking care of each other. Our department has a unity of mission built on a foundation of strong relationships, so we have done very well.
I also have the privilege of serving as medical director at Carol Woods Retirement Community. Working with the leaders there is and remains a pleasure as it is proactive and well-led with a community of residents who appreciate the great efforts that have been made to keep them safe.

Q: What is your day-to-day like?
A: I drive or bike to work every day rather than work from home. Being in my office in the Family Medicine Center helps me stay connected, focused, and productive. Most of my day is in front of the computer, managing the many issues that come to me via email. I also spend hours in WebEx virtual meetings with faculty and department or institutional leaders. My office is fitted with a large video screen, so it is truly a larger-than-life experience.
Q: What challenges have you faced?
A: We faced many challenges when this all started in March, all of which we handled in a calm, thoughtful manner. One decision we made early on was to put our providers into “pools,” to reduce movement across our many clinical settings. We assigned providers to work exclusively in the hospital, on labor & delivery, at occupational health, or in the Family Medicine Center. This was very effective and reduced exposures while providing clarity of roles as our usual operations and schedules were significantly changed.
Another big challenge was the transformation to virtual care and telemedicine. We had been dabbling in this for more than a year so were somewhat prepared, but these methods of patient care were drastically increased and improved in real time. We remain very aware that this is a big change for our patients, too, and are impressed by the spirit of patience and togetherness that we all share. We are grateful to our clinic staff who continued their duties while adjusting to the many changes and have played a critical role in ensuring that our patients continue to have access to their primary health care teams.
Another challenge was moving our inpatient service from the main hospital in Chapel Hill to the UNC Hospitals campus in Hillsborough. We had planned to do this in June anyway, but the COVID-19 crisis necessitated an earlier move. Our faculty and resident physicians did an amazing job of moving our service in early April, and it has thrived. We have transformed Hillsborough Hospital into a busier hospital with a wider range of inpatient services while maintaining outstanding care to our patients and an excellent learning environment for our resident physicians.
Q: In your opinion, what role has Family Medicine played throughout the pandemic crisis?
A: Family Medicine has performed in its usual manner of being innovative, versatile, flexible, and comprehensive. We are leaders in Virtual Care and TeleHealth, while continuing to offer in person care and urgent care in the Family Medicine Center. We have a robust inpatient service in the hospital, we attend the deliveries of hundreds of women and care for their newborns, and we staff the Chatham Hospital inpatient service and emergency room. In addition, our physicians staff UNC Hospitals Occupational Health, the Orange County Health Department, the Town of Chapel Hill, Carol Woods Retirement Community, the North Carolina Farmworker Health Program, and various clinics in the Piedmont Health Services clinics. Every one of these roles was profoundly affected by the COVID-19 crisis and without exception we made the necessarily adjustments to continue safe, high quality care to our patients.
And that is only the clinical part of our department! Many of our faculty are education leaders in the UNC School of Medicine and have had to innovate to continue the education of our medical students and other learners. We also have a robust research program and our researchers have continued their work without disruption, including new initiatives related to COVID-19, such as studying the effect of the crisis on the transition to value-based care. Our Tobacco Treatment Program is part of a consortium of 15 Comprehensive Cancer Centers investigating associations between smoking and COVID-19.
Q: Do you have other personal reflections or comments?
A: Most people have coped surprisingly well in this bewildering time and have adjusted readily to virtual meetings and virtual health care. There are coworkers that I interact with virtually almost every day but, in fact, I have not seen them in person for months. It is all a bit surreal. However, I am confident that we will continue to make the necessary adjustments and are poised to use the lessons learned from this pandemic to improve health care in our community, our state, and our nation.
Q&A with Dr. Evan Ashkin, Director of NC Formerly Incarcerated Transitions (FIT) Program

Evan Ashkin, MD, is a professor of family medicine. He teaches in the underserved track of UNC Family Medicine’s residency program, as well as seeing patients at Piedmont Health Services, which serves vulnerable populations. Dr. Ashkin founded the Formerly Incarcerated Transition (FIT) program to help chronically ill former prisoners who have recently been released connect with primary care medical services that they can access regularly. His team has been working diligently to assist with early releases in the midst of COVID-19.
What role is the FIT program playing in response to COVID-19?
The NC FIT Program has created a new program called “FIT Connect” to address the struggles of medically vulnerable people that are being released from incarceration during the COVID-19 pandemic. We are working closely with the state prison system to assist people in an early release program, connecting to essential health services throughout the state. So far we have received over 240 referrals. We have an amazing team of staff, including Jenny Jones and a number of volunteers from the medical school and undergraduate campus. Hannah Baker, our program manager, is leading the efforts.

What challenges are you and/or your clients facing?
Our clients are facing enormous healthcare challenges and problems with housing and finances. Additionally, they are almost all uninsured, even if they had Medicaid, it is terminated during incarceration and systems are not in place to turn it back on urgently. We also struggle with outreach and communication since many do not have cell phones upon release. This further impedes connections to healthcare and telehealth. We have been successful in securing some funding to cover medical visit copays, pharmacy copays and even to buy phones and phone plans.
In your opinion, what role has Family Medicine played throughout the pandemic crisis?
Family Medicine has again demonstrated a commitment to the well-being of our society and community, and enormous flexibility and creativity in responding to the challenges the pandemic has created.
Do you have other personal reflections or comments?
More than ever, the pandemic has shone a bright light on the numerous deficiencies in our social safety net for vulnerable and marginalized populations. Additionally, it has brought into sharp relief the impact of structural racism throughout our society and medical system, with the terrible disparities in health outcomes from COVID-19 in communities of color.
Family Medicine Medical Student Education
 “As we are working hard to get our students back in the clinical environment I am continuously impressed with their flexibility and creativity. For the past month I helped direct a telehealth elective where groups of students helped patients access video visits, performed outreach to high risk marginalized populations, and helped establish protocols for outpatient telehealth in several different settings. Not only are our students interested and willing to help out, they are working alongside residents and attendings, creating and refining best practices for this new way of delivering healthcare.”
“As we are working hard to get our students back in the clinical environment I am continuously impressed with their flexibility and creativity. For the past month I helped direct a telehealth elective where groups of students helped patients access video visits, performed outreach to high risk marginalized populations, and helped establish protocols for outpatient telehealth in several different settings. Not only are our students interested and willing to help out, they are working alongside residents and attendings, creating and refining best practices for this new way of delivering healthcare.”
–Kelly Bossenbroek Fedoriw, MD, Family Medicine Director of Medical Student Education
Medical student education has undergone significant upheaval, with in person classes and clinic experience not being a possibility. Students have been engaged in electives and didactics for telemedicine and have recently begun to take part in virtual clinics.
At family medicine we have been using student volunteers to staff our parking lot triage, where patients are checked for symptoms of COVID-19 before going into the clinic. Students are happy to help and staff and patients have expressed their gratitude. Our FIRST students (accelerated med school curriculum with students going into our Family Medicine Residency) have been active in volunteering; for example, Alex Gregor has been making masks with providers in Siler City and taking online Spanish and Medication Assisted Treatment training.
All UNC med students are participating in a COVID elective, learning about the biology of the disease as well and societal impact and ethical considerations.
We asked Bailey Minish (FIRST student) and Caroline Fryar (SOM Class of 2021 volunteering in clinic who is planning on being a Family Medicine doctor) about how COVID has affected their learning:
Bailey Minish, FIRST Program Class of 2020:

COVID-19 has affected the way that I have been able to finish up my final year of medical school. I was in the “Transition to Residency” course in March when the university made the decision to transition to online classes and medical students were pulled from clinical rotations in order to conserve PPE and protect students. Many of my learning experiences were transitioned online while other in-person events were outright cancelled. Learning opportunities were provided virtually and included a special course on COVID-19. The university did an excellent job putting together this comprehensive course on short notice that educated medical students at all levels on the current pandemic.
COVID-19 has also affected other important rites of passage at the end of my medical school career. Match day, Skit night, College cup and graduation have all been either cancelled or made virtual. I feel fortunate that since I was already graduating this year, the pandemic has not affected my learning as much as it has for others, but it is still disappointing to miss out on these other important ceremonies.
With all this unexpected free time and with my unique position as a medical student and rising Family Medicine intern, I have tried to find ways to give back to the community. I have been re-learning how to sew and have made reusable cloth masks to donate to various organizations including NC farmworkers and victims of domestic violence. I have done a couple shifts at Piedmont Health Services scribing for providers who are doing COVID-19 testing. I am just now starting to help with the efforts lead by other medical students to do follow-up calls for patients recently tested for COVID-19 through PHS. I have also been involved with Wakebrook Primary Care calling patients with chronic conditions for routine check-ins. I have been in awe of the initiative that my medical school colleagues have taken to help the community; my classmates are involved in making face shields, conducting food drives, helping providers don and doff PPE, and partnering with local agencies to deliver food and provide other services to the elderly. UNC Medical Students are stepping up in a big way!
I am in such awe to see how the community has come together in support of each other in these unexpected, uncertain times.
Caroline Fryar (UNC SOM Class of 2021):
I’m finishing up my Master’s in Public Health so my education hasn’t been seriously derailed in the way that the medical school has been. I found myself really missing medicine, so I signed up for the COVID Elective at the med school. It made my April a little busier than it would have been otherwise, and it wasn’t clinical time, but I’m glad I did it, if only for the connection back to the SOM community. One of the assignments was to write a reflection on a way we’ve been serving, so I attached that here.
Caroline Fryar reflection on volunteering at the Family Medicine Clinic in parking lot patient triage:
“As someone who was repeatedly told on the wards to speak up, project more confidence, and act more decisively, even I am surprised that, for the past three Monday mornings, I’ve pulled on size XS scrubs, driven to the Family Medicine Center and worked as a bouncer.
Well, not a bouncer, exactly—the name of the position is “parking lot triage”—but my job is to stand by the door and screen every person who comes into the building for any symptoms of COVID: fever, cough, shortness of breath. “Well, sure, I have a cough,” one woman says the first week, “but I’m a smoker, I always cough.” So sorry, please wait in the car. “I mean, doesn’t everyone have upper respiratory symptoms right now? With this pollen?” I’m sure you’re right, but let’s have you talk to a doctor by phone in the car, first. I’m a human version of the immune system, keeping virus at bay by telling patients and family members with coughs and runny noses to please wait in their cars.
On the first day, I arrive early, to be oriented by phone. “You know,” says Dr. Bossenbroek Fedoriw, “before we had students out doing this, it was an attending who had to stand in the parking lot. It really frees us up.” It’s an encouraging thought—I’m doing this so Dr. Thomas can spend her time seeing patients—and I’m warmed by the feeling of invisible camaraderie. Later, Dr. Halpert comes outside to see how I’m doing. “The Medical Assistants and people at the front desk,” she says, “you know, they feel so much more safe and comfortable when there’s someone out here to screen patients before they come in. I hope you know what a big difference this makes.” That’s when I make the mental shift from framing my job as being a bouncer to being a protector, although it’s still hard to stand in the clinic doors and turn people back.
The patients who get by me are the avowedly asymptomatic—and I try not to think about the asymptomatic carrier rates as they walk in. Given that the majority of outpatient visits have switched to telehealth, the patients who still come to clinic have visits where an in-person visit is unavoidable: the baby needs a vaccine, or an adult needs a blood draw or a sensitive exam. Patients, too, have learned what questions to answer as they approach any medical building. “No cough, no fever, no shortness of breath, no travel, no COVID,” one says, approaching me. “I know the litany.” “Thanks for wearing a mask!” I chirp. “Remember to sanitize your hands!”
Once, I can’t help myself, and ask a patient what book she’s brought with her. She smiles and holds up a Gallimard edition of La Peste. “I read this in high school!” she laughs.
By the third week of this, protocols have changed—there’s no respiratory clinic, and everyone’s being sent to the RDC. The set of questions I ask has been codified and laminated, pinned at the back of the clipboard. We’re beginning to understand that this state of affairs, while subject to change, will be a months-long haul. The marathon nature of this effort weighs on me. It’s one thing to volunteer in the fever pitch of enthusiasm, looking for some action to take. However, the endurance that’s required to sustain a public health effort like this—both from the provider side, and on the part of the public—is something that’s long been out of practice for most of us. I ask myself, how many more Mondays am I willing to sign up for? The answer is always, “one more,” which is how anything else is accomplished: day by day, and one step at a time.”
Q&A with Linda Myerholtz, PhD, Director of Behavioral Health Education

The following is a Q&A session with Linda Myerholtz, PhD, Psychologist, Associate Professor, and Director of Behavioral Health Education. Dr. Myerholtz sees patients in our clinic and is interested in behavioral health, stress management, wellness and resiliency, mood disorders, anxiety, eating disorders, substance use concerns.
Q: Can you please give a brief description of how your role has changed due to COVID-19?
A: The request for mental health support has been growing as we all experience increased stress due to the pandemic. This is linked to increased worry about the health and safety of ourselves, family and friends, financial stress, inability to engage in many of the activities that we have found meaningful in the past and social isolation. Given this, I have been spending much more time providing mental health therapy services. In addition to an increase in new referrals, many former patients have been contacting me to resume mental health care. I have also been offering emotional support sessions for our clinic staff and interns. All of this is being done by phone or video conferencing.
Q: What is your day-to-day like?
A: I will admit that I love the short commute to my “office” (walk downstairs) and my office mates are lovely (dogs Sophie and Ginger), but I truly miss the regular interactions with our Family Medicine staff and clinicians. My typical day is now engaged in offering mental health therapy services by phone or video for 5-8 hours per day. The rest of my time is spent in time supporting colleagues, video meetings for project collaboration and working on how to adapt the behavioral health curriculum for our learners in the context of most service being provided virtually. This has been a significant challenge.
Q: What challenges are you facing?
A: Like many others, I am missing the regular face to face interactions with co-workers, friends and my patients. While I am very glad to be able to offer phone and video sessions, the technology still has glitches and the interactions are not the same as when we can be in the same room. That being said, being able to offer virtual visits has been very helpful in reducing barriers to care that many people face such as transportation, time for travel, child care, time away from work, etc.
Q: In your opinion, what role has Family Medicine played throughout the pandemic crisis?
A: At Family Medicine, we moved very quickly to be able to offer virtual care visits to patients. It was critical to us that patients continue to receive care that they need in a safe manner. We have been a source of consistency and stability in many patient’s lives. I am so proud of how our staff, clinicians and clinic leadership have responded to ensure continuity of care for our community while also working to keep everyone as safe as possible.
Q: Do you have other personal reflections or comments?
A: This has been a time that has mandated us to move rapidly forward with providing healthcare in innovative ways. We are all learning how to adapt and practice flexibility. We have the opportunity to really reflect on what is most important to us in our lives. We also have the opportunity to “change for the better”, offering each other more compassion and kindness, recognizing that we are all part of a common humanity.
UNC Family Medicine Residency
The Family Medicine Inpatient Service, where our residents are trained in the care of hospitalized patients, was moved from the main hospital in Chapel Hill to the UNC Hillsborough campus in April. This move was accelerated from its anticipated date in June due to the needs of UNC Health in its response to COVID-19. Residents continue to also be stationed at the Main Hospital, where we manage and staff an active, robust Maternal Child Health service.
In outpatient care, due to COVID-19 our residents are seeing patients in a limited capacity for urgent, acute, and maternity care in clinic. For non-urgent care, we have received fantastic feedback as to how they are adjusting to “virtual” visits both via phone and video, online learning modules, and virtual conference and feedback sessions with their faculty preceptors.
 Victoria Boggiano, Residency Class of 2021:
Victoria Boggiano, Residency Class of 2021:
“So much has changed, but largely in a good way. I have been really impressed by how quickly the Family Medicine Center adapted to a virtual care model during the COVID pandemic, with in person visits being reserved for more acute issues. There is great support provided by our faculty to become adept at assessing a patient’s symptoms via telephone or video. I definitely think that it has enhanced my clinical skills!
One of the hardest things about doing inpatient medicine right now is the visitor restrictions imposed on patients. That they can’t have loved ones with them under most circumstances, although completely understandable in COVID times, is really hard. Thankfully Hillsborough has great FaceTime capabilities for family members with iPhones. But I know our patients will be thankful when normal visitation can resume.”

Q&A with Dr. Amir Barzin: Respiratory Diagnostic Center
The following is a Q&A session with Dr. Amir Barzin, a Family Medicine physician who is currently serving as Incident Commander at one of UNC Health’s 11 Respiratory Diagnostic Centers (RDCs). Dr. Barzin temporarily left his role as Medical Director of the Family Medicine Center to assist in leading the RDC during the pandemic crisis. He is a faculty member and graduate of the UNC Family Medicine Residency Program.
Q: What is your current role within UNC’s response to COVID-19?
A: Myself and Dr. David Wohl from Infectious Diseases are the two physicians leading the Respiratory Diagnostic Center at the ACC. Dr. Wohl is the Medical Director overseeing guidelines from the infectious disease standpoint, while I serve as the Incident Commander overseeing day-to-day operations. We are doing both testing and evaluation of people with respiratory complaints for the healthcare system. We have 11 RDCs setup across the area. We’re working to keep people in clinic safe by routing all respiratory complaints to one place. One of the most notable roles we are playing is we are doing more tests at our site than anywhere else in the healthcare system.
Q: What is your day-to-day like at the Respiratory Diagnostic Center?

A: Mainly it’s working with and managing a large team. Our team is amazing, we are all from different departments and areas of work. We have nurses, medical assistants, nursing assistants – everybody working together to provide the best possible care we can. We have a daily huddle every morning to go over everything as a team, including quality checks and assessments. We also have a Safety Officer monitoring PPE and making sure everyone is being safe. Of course we’re helping the healthcare system with testing, but we’re also helping with research projects. We have a couple projects using the RDC as a research site to work with patients and frontline workers, investigating things like plasma and other potential treatments.
Q: In your opinion, what role has Family Medicine played throughout the pandemic crisis, at UNC and more broadly?
A: Family Medicine has really stepped up to the plate during this crisis. We have the unique capacity to see all kinds of people, from kids to adults. Our ability to work in multiple settings has truly been helpful. For example, we are helping lead the charge through actions like moving our inpatient service line to Hillsborough’s campus ahead of schedule, and running Chatham Hospital’s ICU and Emergency Room like we always do. We have a lot of flexibility in our roles that allows us to care for people across the board. Anywhere COVID-19 is interfacing with healthcare, you’ll find Family Medicine.
Q: What kind of impacts do you foresee this pandemic having on healthcare in the future, specifically Family Medicine?
A: We’ve really accelerated our work in they way we’re delivering care. To highlight what we’ve done with virtual care, that’s really important and shows how we’re breaking down the walls and barriers to how we provide care for people. Another thing we are poised to do well is advocate for patients at multiple levels, no matter where they are in the healthcare system. In the future, we’re going to have this opportunity to work together with healthcare leaders to further explore things we’re implementing now like virtual visits, drive-up labs, and other potential ways to improve the patient experience down the line.