

Vibhor Krishna, MD
Vice Chair, Inpatient Operations
Service Line Leader
Associate Professor
A seizure is a brief, strong surge of abnormal electrical activity that affects part or all of the brain. A seizure can cause convulsions or loss of consciousness, and more subtle symptoms such as blank staring, lip smacking, or jerking movements of the arms and legs. In addition to epilepsy, seizures can also occur from high fevers, infection, alcohol and drug use, certain medications, or other medical conditions.
A single seizure does not mean that a person has epilepsy. Often, adult patients with epilepsy have the same type of seizure and symptoms during each episode. Epilepsy is two or more recurrent unprovoked seizures (chronic) from an underlying neurological condition. If you think you have had a seizure, contact your primary care provider right away.
UNC Epilepsy Center is committed to providing high quality comprehensive epilepsy care to patients in North Carolina and the Mid-Atlantic region. The UNC Epilepsy Center is designated as a level 4 epilepsy center, the highest designation, by the National Association of Epilepsy Centers. UNC Neurology and UNC Neurosurgery offer the most complex forms of diagnostic evaluations and treatment options for both adults and children with epilepsy.
The UNC Epilepsy Center has a Epilepsy Monitoring Unit (EMU), a specialized inpatient unit designed to evaluate, diagnose, and treat seizures using state-of-the-art continuous video-EEG monitoring technology. Patients may come to UNC’s EMU for diagnosis of typical spell or seizure, localization of seizure, or anti-epileptic medication adjustment.
The treatment for epilepsy includes both medication and surgical intervention. Medication is the most common treatment method for epilepsy and can effectively control seizures for a large majority of patients.
The benefit of being evaluated at the UNC Epilepsy Center is our patients are evaluated by our multidisciplinary epilepsy team that includes cognitive and behavioral specialists, neurologists, and neurosurgeons. Patients are first evaluated by a neurologist. If a patient is a potential candidate for surgery, the patient is then referred to a neurosurgeon at the UNC Epilepsy Center for evaluation.
UNC’s epilepsy specialists treat over 2,000 patients with epilepsy annually.
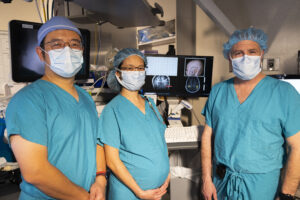
 UNC Health’s Level 4 Epilepsy Center offers Laser Interstitial Thermal Therapy (LITT) to treat both adult and pediatric patients with epilepsy.
UNC Health’s Level 4 Epilepsy Center offers Laser Interstitial Thermal Therapy (LITT) to treat both adult and pediatric patients with epilepsy.
Traditionally, resection or neurostimulation were the available surgical treatment options for epilepsy patients that did not respond to medication. Resection is open brain surgery to remove a diseased portion of the brain. Neurostimulation requires the surgical implantation of electrodes to help detect when a seizure may be starting. Neurostimulation is typically not available to pediatric epilepsy patients.
LITT is a minimally invasive procedure that is just as effective as surgical resection without the risks associated with open brain surgery. Resection typically requires a surgical incision of 20-25 cm, while LITT only requires a 2 cm incision in the skull. Patients treated by LITT also have a shorter stay in the hospital and faster recovery time.
LITT is an appealing surgical option for pediatric epilepsy patients and their families. Children can be seizure-free without needing open brain surgery. Recovery time is also much quicker, allowing the child to resume normal activities much quicker than if they had been treated by surgical resection.
The goal of surgery is to completely stop the seizures or to decrease the frequency and severity of the seizures.
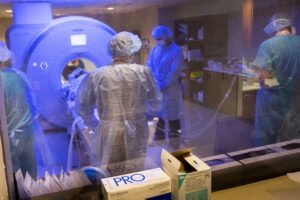
The patient is first brought to the OR where accurate placement of the laser fiber is done using an advanced surgical navigation system. The patient is then brought to MRI where the neurosurgeon activates the laser to burn the diseased tissue. MRI imaging allows the neurosurgeon to follow the progress of the lesion with precision.
Once the patient is brought to MRI, the procedure takes about an hour, compared to resection which typically takes around four hours. The patient is then kept overnight for monitoring before being discharged the following day.
If you would like to make an appointment with one of our neurosurgeons, please call 984-974-4175 to schedule.


Vice Chair, Inpatient Operations
Service Line Leader
Associate Professor


Division Chief, Epilepsy
Medical Director, EEG Lab
Professor, Neurology


Assistant Professor, Neuropsychology


Nurse Practitioner


Assistant Professor, Epilepsy & Clinical Neurophysiology


Assistant Professor, Epilepsy & Clinical Neurophysiology


Program Director, Child Neurology Residency
Associate Professor, Child Neurology and Epilepsy
Co-founder & Clinical Core Leader, UNC Epilepsy Neurogenetics Initiative


Assistant Professor, Neuropsychology


Division Chief and Director of Pediatric Neurosurgery
Children’s Hospital Operating Room Medical Director, Surgeon-in-Chief
Professor


Assistant Professor of Radiology, Neuroradiology


Assistant Professor, Child Neurology and Epilepsy
Child Neurology Residency Leadership Panel
Co-founder & Research Core Leader, UNC Epilepsy Neurogenetics Initiative


Associate Professor, Child Neurology & Epilepsy


Director, Pediatric Epilepsy Monitoring Unit
Assistant Professor, Child Neurology and Epilepsy