Program Overview
The UNC Adult Neurology Residency Program is a four-year (PGY-1 to PGY-4), categorical training program which all 4 years are spent at the main UNC Medical Center and our outpatient clinics. Currently we are matching seven residents per class.
Program by Training Year
PGY – 1
Your intern year is spent primarily with the Internal Medicine Department where you will join other categorial program interns, preliminary program interns, and internal medicine interns.
| Rotation: | Total Duration: |
|---|---|
| Internal Medicine | 32 weeks |
| Emergency Medicine | 4 weeks |
| Neurology | 8 weeks |
| Psychiatry | 4 weeks |
| Vacation | 4 weeks |
PGY – 2
Your PGY-2 year is the first year as a primary neurologist. This is largely focused on inpatient neurology and learning the fundamentals of common neurologic disorders. You will also start your longitudinal resident clinic where you will follow your own primary patients throughout the duration of your residency. We employ and X+Y model for the PGY-2 schedule to allow for dedicated inpatient weeks separated by dedicated outpatient weeks.
| Rotation: | Total Duration: |
|---|---|
| Inpatient Neurology (General Wards, Stroke Wards, Consults) | 20 weeks |
| EEG | 4 weeks |
| Child Neurology | 4 weeks |
| Clinic Rotation | 8 weeks |
| Elective | 4 weeks |
| Neuro Intensive Care | 4 weeks |
| Night Float/Jeopardy | 4 weeks |
| Vacation | 4 weeks |
PGY – 3
This year focuses on developing your subspecialty interests by rotating through the subspecialty clinics and growing more independent in neurologic practice. You have the opportunity and space to do dedicated scholarship electives in research, education, global neurology, or procedural subspecialties.
| Rotation: | Total Duration: |
|---|---|
| Inpatient Neurology Senior (General Wards, Stroke Wards, Consults) | 8 weeks |
| Night Float/Swing | 12 weeks |
| Child Neurology | 4 weeks |
| EMG or Scholarly Elective | 12 weeks |
| Clinical Elective | 12 weeks |
| Vacation | 4 weeks |
PGY – 4
You return to the inpatient services as a senior and focus now on learning how to lead teams, teach, and be the primary decision-maker in the management of neurologic patients. Your attendings will continue to be there for assistance and additional teaching, but the goal is to grow into fully independent and excellent in clinical practice.
| Rotation: | Total Duration: |
|---|---|
| Inpatient Neurology Senior (General Wards, Stroke Wards, Consults) | 16 weeks |
| Night Float/Swing | 12 weeks |
| Child Neurology | 4 weeks |
| Clinical Elective | 16 weeks |
| Vacation | 4 weeks |
Curriculum
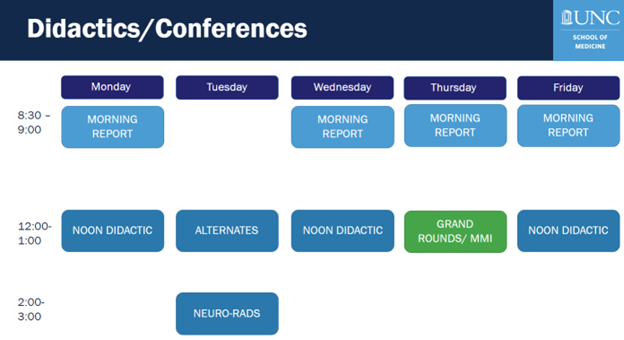
Noon Conference (Monday, Wednesday, Friday): We utilize a rotating block curriculum so that a total of 9 subspecialty lecture series will be covered per academic year. Noon conferences are offered in a hybrid model of in-person and virtual to allow our outpatient residents to attend lecture.
Morning Report (Monday, Wednesday, Thursday, Friday): Opportunity for the inpatient services to share each other’s interesting cases. Facilitated by the senior residents, it is an opportunity for our junior residents to practice the art of localization and differential development.
Resident Teaching Conferences: Twice monthly including Localization Series and Board Review
Professional Development Series (Monthly): Specialty topics relevant to career development and practice with sessions on teaching as a resident, time management, building a curriculum vitae, research as a resident, advocacy and more.
Neurology Grand Rounds: UNC Neurology faculty and invited guest lecturers on innovations and best clinical practice in Neurology.
Neurology Boot Camp and Simulation Series: PGY-2 specific series during July and August to bring you back into the great big world of Neurology. Includes live stroke code simulations, rapid response simulations, LP training, and intensive learning in acute care neurology, common clinical questions, and interactive quiz show.
Neurology Facilities
UNC Medical Center
- 950 Acute Care Beds
- Level 1 Trauma Center
- State’s Burn Center
- ED visits: 75,000 adults annually
- Hospital Admissions: 38,000
- ~ 800 ACGME Residents/Fellows
Neurology Service Line
- Dedicated Neuroscience Floor – 36 Beds
- Dedicated Neuro Intensive Care Unit – 22 Beds
- Intermediate Step Down Unit – 18 beds
- Inpatient Neurology Admissions ~1000/yr
- Inpatient Neurology Consultations ~ 2000/yr
- Resident Clinic saw ~3300 clinic appointments (That’s 160 appointments per resident per year!)
Resident Scholarship
All our residents engage in scholarship during the 4-year program. There are a variety of opportunities for resident scholarly work which include but are not limited to Education/Teaching, Research, Quality Improvement, Diversity, Inclusion and Health Equity. Our residents deliver a minimum of two department presentations: one morbidity mortality conference and one grand rounds presentation.
The Adult Neurology Boot Camp
The Adult Neurology Boot Camp is designed to introduce important principles of neurological care to newly minted PGY2 neurology residents and to help them transition into junior neurology resident status.
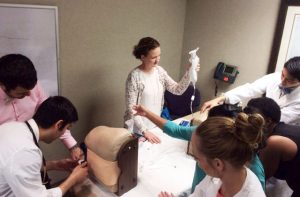
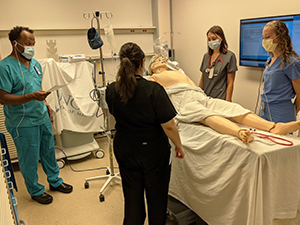
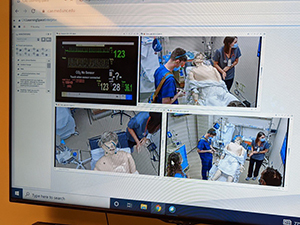
The boot camp lasts two summer months (July and August) and is completed with lectures, interactive clinical case sessions and hands-on labs. Each week is dedicated to a different aspect of neurological care: general neurology, stroke care, neurological intensive care and the challenges of initial night shifts in a hospital. The boot camp covers such topics as neurological exams in adult and pediatric populations, neurological emergencies, MOCK acute stroke exercises, LP simulator lab experience, common neurological consults and neuroimaging.
The camp culminates with a Jeopardy day and a pizza party to celebrate the hard work and the steep learning curve of our junior residents.

Visiting Professors at UNC Department of Neurology

The UNC Department of Neurology is committed to excellence in resident training and education. To support this mission, UNC Neurology visiting professors are invited throughout the year to speak at Neurology Grand Rounds, and to spend time with residents and faculty in informal settings during dinner and the resident noon conference.
The academic year 2019–2020 was unusual due to the pandemic, but we still enjoyed Dr. Jose Gutierrez from Columbia Medical Center who presented grand rounds on “The role of brain arterial dilation in Alzheimer’s disease.” Later over dinner, he led a candid, fun, thought-provoking and inspirational discussion with the residents, followed by a noon conference on career development and importance of critical thinking the next day.


