Curriculum
The Department of Emergency Medicine provides a variety of formal and informal educational opportunities for its members. We strongly believe in the pursuit of education allows our residents to mature in both their professional and personal lives. Concepts of clinical management, the approach to differential diagnosis, problem-solving, and integration into the institutional system are obtained through conferences, meetings, journal club discussions, and clinical supervision in the emergency department. Educational resources are readily available for resident access through web-based textbooks and applications, such as AccessEmergencyMedicine. Topics for all aspects of the educational experience are based upon established standards of emergency care, recurrent or unusual emergency department cases, new developments in subspecialties related to emergency medicine, and interdisciplinary approaches to patient management.
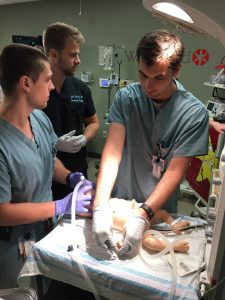
Simulation Lab
Didactics
Resident conference is one of the highlights of the UNC EM experience. The curriculum is managed by Dr. Maglin Halsey-Nichols, as well as the chief residents.The resident conference is held weekly on Wednesday mornings at the UNC main campus. On the first Wednesday of the month, our resident conference it held at the WakeMed campus and involves a hands-on simulation session to facilitate our learning. Each month is a new module, with core modules covered on an annual basis and additional modules rotating every other year. We strive to balance traditional didactics with interactive, hands-on learning and simulation. Conference content is created by residents of all years as well as UNC EM faculty, UNC faculty from collaborating departments, and educators from around the country. First-year residents each present on ultrasound topics, while second-years lead the residency in discussions of controversial topics within emergency medicine. Third-years provide core content review as a part of a recurring series. Other popular conference segments include Worst-Case Scenarios (residents and attendings guiding learners through their toughest cases), Wilderness Medicine Day (held at a local state park), and interactive review using the online platform Kahoot. Resident conference is also when mortality and morbidity review takes place. Additionally, we utilize conference time to bring internationally-recognized speakers in front of the residents for expert content talks, often in a virtual format. Recent speakers have included Amal Mattu, Corey Slovis, and Ben Wachira. Finally, we draw on numerous resources for robust asynchronous learning to supplement our conference experience, including content from ALiEMU, EM:RAP, and EM Cases. Our frequent Journal Club also offers an outlet for asynchronous learning. With all these opportunities, it is no wonder our residents have scored some of the highest marks on the In-training Exam.
Concentrations
During the PGY-2 year, residents declare a concentration within EM, an area they are passionate about and hope to incorporate into their career. Areas include, but are limited to, medical education, research, administration, EMS, geriatrics, pediatrics, toxicology, and global health. Through this program, residents are paired with expert faculty and introduced to supplemental training, leadership opportunities, and scholarly projects. For example, a resident may select EMS as their concentration and participate in field training or disaster drills with local EMS providers and police.
Learn More
Clinical Rotations
PGY 1 Year
The first year of training begins with a 2-3 week orientation in mid-June which presents the basics of emergency care. A full schedule of clinical experience, ATLS, PALS and orientation lectures is provided. Orientation lectures includes an airway management course, procedure labs, and an introduction to ultrasound. We also provide free time and social events to allow new residents to get settled and acquainted. Clinical experiences focus on management of critically ill patients in several intensive care settings, obstetrics, utilizing ultrasound in the emergency department, and a heavy emphasis on procedural skills. EMS experiences will be incorporated into your EM months in different ways.
| Rotation: | Duration: |
|---|---|
| Orientation | 2 Weeks |
| Emergency Medicine | 31 Weeks |
| Ultrasound/Anesthesia | 4 Weeks |
| Obstetrics | 4 Week |
| Neurosurgical Intensive Care | 4 Weeks |
| Medical Intensive Care (UNC) | 4 Weeks |
| Vacation | 4 Weeks |
PGY 2 Year
The second year curriculum focuses on consolidation of the fund of knowledge acquired in the first year. This year incorporates a higher level of management of critically ill adult and pediatric patients, orthopedics, and trauma. Second-year residents are expected to take on an increasing level of responsibility in the emergency department.
| Rotation: | Duration: |
|---|---|
| Emergency Medicine | 32 Weeks |
| Trauma | 4 Weeks |
| Pediatric Intensive Care * | 4 Weeks |
| Medical Intensive Care (WakeMed) | 4 Weeks |
| Orthopedics | 4 Weeks |
| Vacation | 4 Weeks |
PGY 3 Year
The third year of training emphasizes increased clinical and administrative responsibilities including resident and medical student supervision, running trauma resuscitations, aeromedical control, and department management. Clinical experiences consist almost exclusively of emergency department rotations with a month of elective time and a month of administrative responsibilities. The resident is expected to complete a scholarly activity, which was initiated during the second year. Each third year resident is given a chief or director role to maximize resident involvement in all aspects of the curriculum. We make an effort to allow all our senior residents to attend ACEP’s Scientific Assembly.
| Rotation: | Duration: |
|---|---|
| Emergency Medicine * | 40 Weeks |
| Elective | 4 Weeks |
| Administration | 4 Weeks |
| Vacation | 4 Weeks |
*EM blocks include shifts at both UNC and WakeMed, including 20% pediatric patients. PGY-1: 19-20 shifts, PGY-2: 18-19 shifts, PGY-3: 17-18 shifts
- UNC Main campus:
- 8-10 hours shifts weekdays, 12 hour shifts weekends
- Team based with 1 attending and 2-3 residents per clinical area
- Senior resident: runs the department; responsible for trauma activations (including all intubations and sharing other procedures)
- Interns: encouraged to challenge themselves and carry appropriate patient loads
- Includes adult and some pediatric shifts and patients
- WakeMed Raleigh campus:
- 10-hour shifts in adult areas, 9-hour shifts in pediatric ED
- Team based with 1 attending and 1 resident, as well as some APP coverage
- Residents: responsible for trauma activations (including all intubations and sharing other procedures) and medical resuscitations
- UNC Hillsborough campus:
- 8-10-hour shifts
- Team includes 1 attending and 1 resident, as well as some APP coverage
- WakeMed North campus:
- 9-hour shifts
- Team includes attending and resident, as well as some APP coverage